Skin cancer is on the rise in many countries around the world, but so are the methods to treat it. Bárbara Pinho reports
Every year, the beaches of the Mediterranean are filled with tourists from the UK and other northern European countries. The annual exodus is driven by the desire for good weather and relaxation. But having a good time doesn’t seem to be enough. According to a survey of British women commissioned by skincare brand Dove in 2021, nearly 60% of respondents said they were happy as long as they returned from their holiday tanned. A good tan has long been a big deal for many people, who see it as a healthy and attractive look.
But the golden look has its drawbacks. Over the years, the UK, like other countries around the world, has seen a worrying rise in skin cancer rates, and sun exposure seems to be one of the reasons behind the increase.
Since the early 1990s, melanoma skin cancer incidence rates have more than doubled in the UK. The latest figures show that there are more than 16,500 new cases of melanoma skin cancer each year – around 46 new cases every day. It’s the fifth most common cancer in the country and projections estimate that the numbers will rise by 9% by the late 2030s. But while rates are increasing across all population groups, this increase isn’t the same across all age groups. Since the early 1990s, melanoma rates have increased by 67% in people aged 25-49, and by an astonishing 236% in those aged 70–79.
‘Ageing is the number one risk factor for cancer. So, with more older people in our population, we’re very much expecting to see more cases of melanoma but also broadly just more cases in cancer,’ explains Beth Vincent, health information manager at Cancer Research UK.
Vincent goes on to explain that there are a number of other reasons why we’re seeing such an increase in skin cancer. People are more aware of the disease and are getting their skin checked more often, which leads to more diagnoses. And then there’s the issue of unsafe exposure to UV radiation.
UV radiation and skin cancer
There are two main types of skin cancer: non-melanoma skin cancer and melanoma skin cancer. Non-melanoma skin cancers, including basal cell carcinoma and squamous cell carcinoma, typically develop in the epidermis, the outer layer of the skin, and are often associated with prolonged exposure to the sun. Melanoma originates in the melanocytes, the cells responsible for skin pigment in the deep layer of the epidermis. It tends to be more deadly and to metastasise aggressively through the body.
While UV radiation isn’t the sole factor behind melanoma skin cancer, it seems to play an important role. ‘The first step, nearly all the time in melanoma skin cancer, is that one normal melanocyte will get a mutation, and this is most commonly caused by ultraviolet light,’ says Dot Bennett, a professor of cell biology at St George’s, University of London in the UK.
If you had a lot of sun exposure when you were young, you set some things in motion that may not be apparent for 30 years
When UV radiation reaches melanocytes, it triggers mutations in their DNA. Mutations in these cells can trigger abnormal proliferation, leading to a tumour. This doesn’t happen overnight, however; UV exposure over the years has a cumulative effect on a person’s skin and tumours can take decades to appear, which is why older patients tend to have more melanoma than younger ones.
‘If you had a lot of sun exposure when you were young, you sort of set some things in motion that may not be apparent for 30 years,’ explains Craig Slingluff Jr, a surgical oncologist at the University of Virginia in the US.
In around 50% of patients, the melanoma tumour cells contain a mutation in a gene called BRAF. This mutation causes certain cell signalling proteins to become overactive, which drives the cells to divide too much. However, recent studies have shown that these mutations do not always cause skin cancer, but instead can result in the formation of completely harmless pigmented moles on the skin.
Moles are clusters of melanocytes that started multiplying and then stopped. But what still baffles scientists is why they stop multiplying in the first place. A proposed explanation for this behaviour is that, once activated, the extra divisions caused by BRAF make these cells ‘sense’ and respond to their own overgrowth. The same kind of sensing is observed in normal tissues as we age and some cells have divided many times. This is called cell senescence.
‘All mammalian cells can undergo cell senescence. It’s a programme of growth arrest where the cell says “No, I’m not going to divide ever again,”’ explains Bennett. ‘If you have any mole, nearly all cells in it are senescent.’ Other aspects of cell biology also help to explain why some people are at greater risk of skin cancer than others.
Why skin cancer affects people differently
Black people have much lower rates of both melanoma and non-melanoma skin cancers because their melanocytes produce more melanin, the skin pigment that protects against UV rays.
Bennett explains that in the skin, melanocytes have branches that touch keratinocytes, the cells that make up the entire outer layer of the skin. Melanocytes produce melanin and use these branches to distribute it to surrounding cells. Melanin enters cells and sits just above their nuclei to protect them from UV radiation. ‘It’s very clever, melanin protects the nucleus like an umbrella,’ she adds.
People with more melanin therefore have more protection from UV. Importantly, this does not mean that people with darker skin tones are immune to skin cancer.
‘There is a common misconception among some individuals that darker-skinned people are completely protected from developing skin cancer,’ says Faranak Kamangar, a dermatologist at the Palo Alto Medical Foundation in the US. ‘However, this belief is not accurate. While it is true that darker skin tones have more melanin, this does not make them completely immune to skin cancer.’
Red-haired people, on the other hand, are extremely sensitive to UV radiation and prone to skin cancer. People with red or fair hair, fair skin and freckles do not tan fully, because of a mutation in the MC1R gene. This mutation makes melanocytes less responsive to UV light and also causes melanin to be a lighter colour and less protective.
But natural skin protection isn’t enough to explain all these skin cancer trends. Behaviour is another key factor in explaining why some people get more skin cancer than others.
Why skin cancer is increasing in the UK
When they were looking at the latest trends around the UK, Vincent and her colleagues at Cancer Research UK noticed some curious numbers. They saw that among people over 55, skin cancer rates were higher in the late 2010s compared with the late 1990s. So a higher proportion of older people are getting skin cancer now than back then. And the exodus to the Mediterranean may be to blame.
‘If we look back to the 1960s or so, there was the big package holiday boom, there were a lot of trends to have tanned skin,’ Vincent says. ‘The link between UV or sun exposure and skin cancer was much less well understood. So, we do think that possibly those trends to have tanned skin and the availability of being able to go abroad and sunbathing […] actually could be what triggered this particular increase in the over-55 age group.’
The British and other northern Europeans’ habit of sunbathing without proper protection when visiting Mediterranean countries partly explains why they end up with more skin cancer. Another explanation lies in sunbeds, which with their high UV index give their regular users a 75% higher chance of developing melanoma.
We’re seeing an increasing trend in incidence of melanoma – but in terms of death, a downward trend
But it is not all doom and gloom across the skin cancer spectrum. Although there are more cases of melanoma across the country, there’s also more survival.
‘Last summer, we saw that melanoma skin cancer cases had reached an all-time high of cases […] but we also actually saw that deaths from the disease were dropping. So, it’s a very mixed picture,’ says Vincent. ‘We’re seeing, in terms of incidence, an increasing trend, but in terms of death, a downward trend.’
Melanoma skin cancer survival has doubled in the last 50 years in the UK. Though there are no survival statistics for each stage of melanoma in the whole country, data from England shows that if melanoma is caught early (stage 1), almost everyone survives their cancer for five years or more after diagnosis. Survival is more difficult for those diagnosed at more advanced stages, but even this picture is changing.
‘For people with advanced melanoma, where it spreads to the lungs, liver etc, 15 years ago the median survival was about 6–9 months. And now it’s at least three years. […] it’s very exciting,’ says Slingluff. The difference between where we were 15 years ago and where we are now is largely due to discoveries in cell biology - discoveries worthy of a Nobel prize.
The rise of immunotherapy
James Allison, an immunotherapy researcher at The University of Texas MD Anderson Cancer Center in the US, met his first patient in New York in 2006. A young woman named Sharon Belvin had been battling stage 4 melanoma for two years. Belvin had done chemotherapy, but it didn’t stop the disease from spreading; at the age of 23, she was told she had only a few months to live. As a last resort, Belvin took part in a clinical trial of an experimental drug called ipilimumab.
Ipilimumab is a type of immunotherapy called an immune checkpoint inhibitor. It works by helping the patient’s own immune system to recognise and destroy a tumour. When cancer cells start to spread, the immune system tries to fight them. However, cancer cells have a way of evading the immune system’s activity. T cells, a type of immune cell that fights threats, have receptors on their surface that, when attached to certain proteins, tell the T cell to stop attacking.
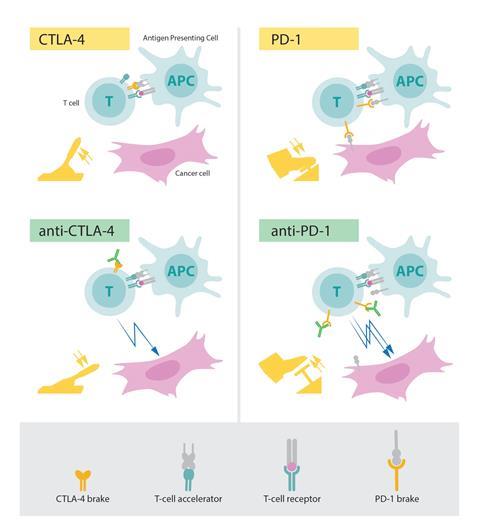
Cancer cells are capable of producing these proteins, which bind to the receptors in the T cell and stop them from attacking the cancer. Immune checkpoint inhibitors such as ipilimumab block the interaction between the receptors on T cells and the proteins produced by cancer cells. This ‘re-activates’ the T cell, allowing it to destroy the cancer cell.
After starting treatment, Belvin’s immune system was able to eliminate the cancer cells. Her tumours started to shrink and eventually disappeared within three months. Belvin went on with her life and has been cancer-free ever since. Over the years, she has shared pictures of her children with Allison, with whom she has become good friends.
Allison is behind the discovery of how CTLA-4, a type of receptor that sits on the surface of T cells, is used by cancer cells to shut down the immune system. His findings led to the discovery of drugs that inhibit CTLA-4, ensuring that T cells do their job and attack cancer cells.
He shared the 2018 Nobel prize in medicine with Tasuku Honjo for their work in cancer immunology. Honjo was recognised for his discovery of another important receptor called PD-1 and its similar role in the immune system. Both discoveries led to the development of CTLA-4 inhibitors and PD-L1 inhibitors, drugs that help boost the immune response against tumour cells.
The clinical use of immune checkpoint inhibitors over the past years has revolutionised how we treat melanoma. These drugs have also paved the way for other immunotherapy strategies to treat the disease, such as vaccines.
‘The fact that checkpoint blockade works is clear proof that immunotherapy can be effective, which was not something everyone believed 15 years ago,’ explains Slingluff.
Vaccines for skin cancer
Cancer vaccines aren’t new. Although there are vaccines that protect against cancer by targeting viruses, such as the human papillomavirus (HPV), the whole concept of a vaccine is difficult to apply to all types of cancer.
Unlike bacteria and viruses, which seem foreign to our immune systems, cancer cells resemble normal and local cells, making them harder to target without harming healthy cells. Each person’s tumour is also somewhat unique and has its own distinctive characteristics, making it even harder to make a vaccine that works for everyone. However, it’s still possible to develop vaccines that somehow give the immune system an edge over the tumour, and this is what Slingluff has been working on for the past few years. He and his team have been looking at multipeptide vaccines.
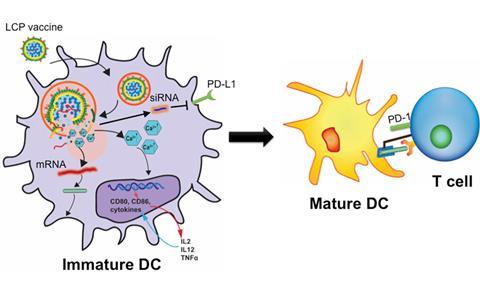
Multipeptide vaccines use multiple peptide fragments chosen for their ability to stimulate the immune system to recognise and attack specific targets, such as cancer cells. ‘What we’re trying to do is to get the immune system to recognise melanoma,’ Slingluff explains. ‘We expose it to certain molecules or fragments of molecules that are present on the melanoma.’
So far, he and his team have tested multipeptide vaccines in 167 patients with high-risk (stage 2 to 4) melanoma. They carried out a trial 15 years ago and kept following the patients ever since. In a recent long-term study, they reported that their melanoma vaccine stimulated different types of immune cells, namely helper T cells and killer T cells. These cells acted against melanoma, prolonging patients’ survival and preventing the cancer from coming back. Although the results are promising, the team is working to find out what exactly is happening at the cellular level that leads to improved survival.
But despite the good results, the melanoma vaccine closest to market is an mRNA vaccine being tested by Merck and Moderna. The companies are conducting a trial in patients with late-stage melanoma who have had surgery to remove the tumour. They’re testing a combination of an mRNA skin cancer vaccine and Keytruda, an immune checkpoint inhibitor drug.
Last year, the results of their phase 2 trials showed that combining the vaccine with the immune checkpoint drug reduced the risk of relapse or death by 49% compared to using the drug alone. They also saw that using both therapies reduced the risk of the cancer spreading by 62%. The trial involved 157 stage 3 and 4 melanoma patients.
The companies are now moving into phase 3 of the trial, which will enrol nearly 1100 patients. The trial was announced a year ago and full results are expected in 2029.
‘If that’s positive [the phase 3 trials], I would expect that [these vaccines] may come to market within a few years,’ says Slingluff. Yet, while medicine has made huge strides in recent years, prevention is still an important step in avoiding skin cancer altogether. ‘Up to nine in 10 cases of melanoma skin cancer could be prevented by being safe in the sun and also avoiding sunbeds,’ says Vincent. ‘We’re talking about the vast majority of cases.’
How do sunscreens work?
People have been caring for their skin long before we put sunscreen in plastic bottles. Traditional herbs and oils have been used to protect the skin since ancient times: the Egyptians used ingredients such as rice bran and jasmine to prevent tanning, while the ancient Greeks used olive oil. The invention of the SPF rating in the 1960s brought the idea of sun protection to consumers around the world.
The active ingredients of sunscreens are classified as either organic or inorganic chemical absorbers. Organic chemical absorbers, such as avobenzone, absorb photons of UV rays and dissipate them harmlessly as heat. Variations in the structure of molecules can lead to absorption at different wavelengths of UV radiation.
Inorganic compounds such as titanium dioxide and zinc oxide act mainly as reflective barriers, although they can also absorb UV radiation and dissipate it harmlessly.
But sunscreens become less effective over time. Some of the chemicals in sunscreen are not photostable and will break down. Exposure to water and sweat also affects the way sunscreen works, so it is a good idea to reapply every few hours.
Skin checks and staying safe in the sun
Most of the guidelines for staying safe in the sun are pretty well known: stay in the shade, especially between 11am and 3pm; cover up with clothing, a hat and UV-protective sunglasses; apply plenty of sunscreen (see box); and make sure you’re using a sunscreen with at least SPF 30. And the advice is for everyone.
‘Everyone should take appropriate measures to protect their skin from UV radiation, regardless of their skin colour,’ adds Kamangar.
As well as staying safe in the sun, it is important to check your skin for any unusual signs. In particular, always look for moles or signs that follow the ABCDE rule: assess whether they are asymmetric, have irregular borders, have varied colours, are larger than 5mm in diameter, and evolve or change over time. Vincent adds that those with brown or black skin ‘might be more likely to see changes on the palms of hands, soles of feet and under the nail or in the nail bed’.
With incidence trends on the rise, staying safe in the sun and knowing how to look for signs of skin cancer can make a difference. And because the risks of UV radiation are cumulative over time, it’s never too late to start taking better care of your skin. For those who go to Mediterranean beaches, making a point of protecting your skin every year could make a difference in the long run. ‘If we start protecting our children’s skin better, then we may have less melanoma when they get to be 30 or 40,’ concludes Slingluff.
Bárbara Pinho is a science writer based in Porto, Portugal


















No comments yet