Is it really worth supplementing your diet with health-boosting pills? Emma Davies reports
Is it really worth supplementing your diet with health-boosting pills? Emma Davies reports
’Eat more fruit and vegetables.’ It’s a message that’s drummed into our skulls day in, day out. On supermarket shelves, food packaging is emblazoned with the ’five a day’ message. And TV nutritionists regularly make hapless volunteers feel like social pariahs for not eating enough of what’s good for them (and too much of what’s not). But many people just don’t have time to monitor their daily portions of fruit and veg, so they take the quick option and buy supplements instead.

And, as a consequence, the supplement industry is booming. Almost three out of every 10 people in the UK currently take a supplement on most days, according to a survey published by the UK Food Standards Agency (FSA) in May. Most of these supplements contain common antioxidants such as vitamins A, C, and E, and provide a shortcut to the five a day option. But in the past few years evidence has emerged suggesting that some of the high dose capsules could do more harm than good.
There is no doubt that a diet rich in antioxidant-containing fruit and vegetables is good for us. Antioxidants are often said to ’mop up’ free radicals, which form when inhaled oxygen is metabolised, producing oxygen free radicals and other reactive oxygen species. The body’s antioxidants can dispose of most of these free radicals but some remain to cause damage, including to DNA. Over a lifetime, the damage can reach a level high enough to cause mutations that initiate and promote cancer.
’There is very good evidence that free radicals are involved in certain diseases, especially cancer and neurodegenerative disease, and reasonable evidence linking free radicals to cardiovascular disease,’ says Barry Halliwell, a biochemist and deputy president in charge of research and technology at the National University of Singapore, who pioneered research into free radicals and disease. ’So why is it that all the people who are taking big doses of antioxidants are not living forever and being protected against all these diseases?’
Miracle or marker?
Scientists were first alerted to antioxidants’ possible protective powers following correlative epidemiological studies. These suggested, for example, that people with high blood levels of the antioxidants vitamin C, vitamin E and beta-carotene have a far lower risk of developing cancer, diabetes or heart disease.
’But is it a fact that people with high blood levels of antioxidants have a lower risk of disease or is it just a marker of the fact that they have a healthy diet?’ asks Halliwell. It’s a question that few have asked - many supplement trials continue to be based on the assumption that antioxidants lower the risk of disease.

Most of the European and US intervention trials comparing antioxidant supplements with placebos have shown no supplement benefits, says Halliwell. Many of the trials have focused on particular disease groups. Randomised beta-carotene trials on smokers in the mid-1990s, for example, found no benefit for lung cancer and two studies actually suggested an increased lung cancer risk in smokers treated with beta-carotene. One of these beta carotene trials, set up in 1992 by researchers at the US National Cancer Institute (NCI), Bethesda, was abandoned two thirds of the way through after it emerged that those taking supplements were at a greater risk of developing lung cancer.
A Finnish trial that ended in 1993 gave male smokers vitamin E and beta-carotene supplements, and the results suggested that beta-carotene caused a 23 per cent increase in prostate cancer cases. Then, in May 2006, an expert scientific panel convened by the US National Institutes of Health (NIH) concluded that there was strong evidence to recommend that smokers avoid beta-carotene supplements.
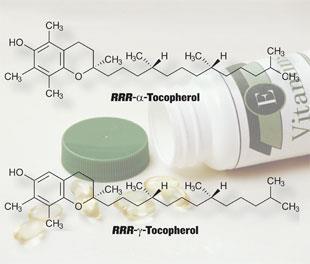
Robert Verkerk, executive and scientific director at the Alliance for Natural Health, a UK not-for-profit organisation that promotes natural healthcare products, argues that synthetic forms of vitamins are considerably different from natural vitamin complexes found in foods. Naturally occurring vitamin E, for example, is a mix of four tocopherols and four tocotrienols but vitamin E supplements used in trials generally contain only alpha-tocopherol. The average western diet contains more gamma-tocopherol than alpha-tocopherol, and Verkerk argues that high doses of the alpha form inhibit the uptake of gamma-tocopherol. ’It’s not really surprising that the trials end up with negative results,’ he says.
Halliwell points to a similar story with beta-carotene. ’A lot of carotenoids are absorbed from fruits and vegetables but if you take big doses of beta-carotene, you actually block the uptake of some of the other carotenoids.’
Dose drama
Many of the intervention trials used high doses of a single agent such as vitamin E or vitamin C. ’A classic misinterpretation in nutrition says that if 10
g of a vitamin is good, 10g must be orders of magnitude better,’ says Halliwell. In reality, most nutrients follow a plateau effect or a bell-shaped curve. ’You get a benefit up to a point then if you eat any more you don’t get any more benefit, or you get deleterious effects,’ he explains.
Indeed, many supplement takers seem to believe that more is better, or simply choose to ignore the possible risks. The FSA survey suggests that almost 15 per cent of the UK population have taken a high-strength supplement in the past year. This is despite the fact that 50 per cent of those who take supplements are fully aware that taking a number of different pills could result in the unintentional consumption of high levels of vitamins and minerals, with possible adverse side effects.
Halliwell is convinced that taking very high concentrations of vitamins could be detrimental to health. ’If you start taking way over the recommended daily allowance [RDA] of a vitamin, you’re moving from nutrition to pharmacology. What we don’t know in humans is what the optimal intake of antioxidant nutrients is. It’s probably not very high - very big doses of vitamins are probably overdoses.’
Recent meta-analyses,combininglarge numbers of supplement trials, have thrown up apparent dangers of taking certain supplements in high doses, with the stark warning in one case being that ’vitamin A, beta-carotene, and vitamin E may increase mortality’. This came from a meta-analysis published in February 2007 by a Danish team led by Goran Bjelakovic at the Cochrane Hepato-Biliary group, part of the Center for Clinical Intervention Research at Copenhagen University Hospital. The team analysed the results of 68 randomised trials comparing beta carotene, vitamin A, vitamin E, vitamin C, and selenium. The first three came out particularly badly while they concluded ’the potential roles of vitamin C and selenium on mortality need further study’.
The researchers did not expect such negative results, reveals team member Christian Gluud. ’The median doses of all vitamins were within current recommended dosages so we were surprised,’ he says. The work obviously had a strong effect on Gluud who has some simple advice regarding vitamin A, beta-carotene, and vitamin E supplements. ’Do not take them, unless a qualified physician recommends you to do so based on a valid diagnosis of you lacking the vitamin.’
In a later editorial in the Journal of the National Cancer Institute , Bjelakovic and Gluud speculate on why supplements may be detrimental to health. ’Reactive oxygen species [ROS] in moderate concentrations are essential mediators of reactions by which the body gets rid of unwanted cells,’ they say. So if antioxidant supplements cut free radical levels, they may interfere with the body’s ability to get rid of damaged cells including those that are precancerous and cancerous. ’High-level antioxidant supplements could potentially upset an important physiologic balance,’ they reason.
They also point out that antioxidant doses that may be beneficial are not known and may differ among individuals. Antioxidants could be harmful in people with lower innate levels of ROS but good for those with high levels, they suggest.

Many experts question the validity of meta-analysis results. Halliwell is one of the doubters. ’A lot of research in the field is funded by the supplement industry, which obviously wants to get results that suggest we should all be taking these things. It may fund 20 human studies and only publish the one that shows positive effects. A huge problem with meta-analysis is that you don’t have access to all the information. All you know is what is published.’
Verkerk is critical of the Danish meta-analysis. The studies included in the analysis rely on very high dosages of pharmaceutical-grade, synthetic forms of supplements, he says. ’The dosages used are typically much greater than those recommended on the labels of food or dietary supplement products.’
But the supplement industry was dealt a further blow last May with the publication of another widely publicised meta-analysis, this one from a team led by Karla Lawson at the NCI. Her team investigated the association between multivitamin use and risk of prostate cancer in almost 300,000 men enrolled in the NIH diet and health study. The meta-analysis apparently highlighted an increased risk of advanced and fatal prostate cancers among men reporting ’excessive use of multivitamins’ (more than seven times a week). In particular they found an increase in advanced prostate cancer with heavy multivitamin use combined with a beta-carotene supplement.
Concerns about the potential dangers of taking high-dose forms of some vitamins have led to calls for more regulation and supplement testing. Halliwell would like to see a higher level of quality control and regulation of supplement marketing.
Bjelakovic and Gluud suggest testing supplements before they come to market. Gluud goes so far as to suggest ’full clinical trials with randomisation of supplements versus placebo’. He is keen to see a higher level of regulation. ’There is too much danger to both healthy and diseased populations by having these unregulated markets,’ he says. ’We simply run the risk of chemical killing fields if we do not regulate such products sufficiently.’
Marking the way forward
There are serious holes in our knowledge of how antioxidant supplements actually work, and more fundamental studies are desperately needed. Biomarkers are a good way of following what is going on in the body. Several years ago, Halliwell’s team started developing biomarkers of free radical damage in the human body, which can be measured in blood and urine.

His team initially used biomarkers to monitor free radical damage in volunteers given high doses of antioxidants. ’Our studies I think were the first, followed by a number of studies from other groups all over the world,’ says Halliwell. In general the biomarker work suggested that if you take healthy, well-nourished people - just the kind of people who are likely to take supplements - and give them high doses of antioxidant supplements, you do not decrease free radical damage.
Next, his team looked at what does decrease levels of free radical damage. ’And it is, interestingly, all the things that we know about. If you measure free radical damage to lipids, for example, obesity, high blood pressure, and high blood cholesterol affect it the most. The best way to bring down your free radical damage is to control things such as cholesterol,’ he says.
Halliwell’s team continues to search for new biomarkers. ’We’re doing experiments where we’re changing people’s diets and looking at what is happening to biomarkers of free radical damage. These are very complex experiments because you can’t double-blind them.’
Susan Fairweather-Tait, a nutritionist from the School of Medicine, Health Policy and Practice at the University of East Anglia, UK, is looking for new biomarkers to monitor how selenium works in the body. This compound is often taken with antioxidants and is a trace element nutrient that acts as a co-factor for the activity of important antioxidant enzymes.
’If you’re marginally deficient in selenium or marginally overloaded, it’s difficult to pick up and you can’t really say whether somebody’s diet is adequate or not, so we need these early biomarkers,’ she says. The new markers use gene and protein expression.
Pill popping
Halliwell does take a daily supplement. ’I take one that has the RDA of all the major vitamins and minerals because I may well miss out on one nutrient,’ he says. ’If you take something that has the RDA it might make up for that and it’s never going to be near a dangerous level.’ Verkerk takes a slightly more complex mix of about 60 food forms of vitamins and minerals derived directly from fruit and vegetables - and a couple of amino acids.
But Fairweather-Tait feels very strongly that you should only take supplements under special circumstances. ’You can very easily have an unbalanced intake of nutrients by taking pills,’ she warns.
Perhaps a way forward is to supplement without pills. Fairweather-Tait can envisage a time when people will buy more foods enriched in certain compounds, such as high-selenium broccoli: ’I’m talking about things that I don’t really approve of but I can see there’s a market there.’ In her opinion, ’nutrition is about making sure that the food supply - the staple foods - is adequate for our needs’. She is working with Harvest Plus, a UK organisation that breeds biofortified food crops, which contain more micronutrients, to improve nutrition among the poor in developing countries. ’Through fertilisation and breeding programmes we can have wheat and other basic food crops that contain more iron, zinc and vitamin A,’ she says. ’Paying attention to the nutritional value of staple food crops is the way forward.’
People in the developed world are already able to get all the nutrients they need from their diet, and yet many still pop vitamin pills daily, so it’s hard to imagine supplements being abandoned altogether. And for most health-conscious consumers, it doesn’t seem to matter that we don’t know exactly how most supplements affect health. We still don’t know why our daily portions of fruit and veg are good for us. They just are.
Emma Davies is a freelance science writer based in Bishop’s Stortford, UK
References
293, 1338
3 E Milleret al , Annal. Intern. Med ., 2005, 142, 37






No comments yet