Want some relief for a cold? A hot spicy curry might be as good as anything, the experts tell Victoria Ashton.
Want some relief for a cold? A hot spicy curry might be as good as anything, the experts tell Victoria Ashton.
Tickly throat? Runny nose? Hacking cough? Feeling generally bunged-up? It’s the cold season again. Typically every year we might get at least one attack of the ’common cold’, with symptoms of headache, runny nose, congestion, sore throat and high temperature lasting from a few days to a few weeks. Although not particularly dangerous, the common cold is widespread - and costly. Businesses in the UK lose an estimated ?1300m every year through sick days because of cold. And we spend over ?100m each year on over-the-counter (OTC) cold remedies. But is there any evidence to suggest that the money we spend on conventional remedies does any good? Or could traditional remedies prove just as effective?
Each symptom of the common cold needs a different type of treatment. Table 1 shows typical constituents of cold remedies. For example, a blocked nose might require either a topical or oral decongestant; a dry cough could require something to suppress the urge to cough and a sore throat might just need a soothing effect or painkillers. Generally cold remedies can be bought as medicines, tablets, lozenges, or soluble powders. Cold remedy ingredients themselves have not changed markedly in the past 50 years or so. But what are we taking when we use a cold remedy, be it cough medicine, decongestants, analgesics, or throat lozenges?
Table 1. Typical remedies for cold symptoms
| Dry tickly cough | Antitussives | Dextromethorphan, codeine |
| Runny nose, sneezing | Antihistamines | Chlorpheniramine, doxylamine |
| Aches and pains, headaches, fevers | Analgesics | Paracetamol, aspirin, ibuprofen |
| Congested nose/blocked sinuses | Oral decongestants Topical decongestants | Xylometazoline, oxymetazoline Pseudoephedrine, phenylephrine, ephedrine |
| Sore throat | Anaesthetic | Benzocaine, benzyl alcohol |
Medicines for a dry or tickly cough usually have some sort of active opiate-based ingredient such as dextromethorphan or codeine within a syrupy mixture. The active ingredient acts on receptors in the brain that may have some role in suppressing coughing. Coughing is a complex process involving a series of reflex events occurring over a timescale of just a few seconds. Neuroscientists still don’t fully understand the exact processes involved and continue to work to try to understand the coughing reflex action.
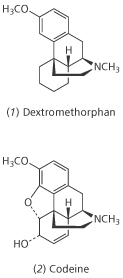
Testing times
Whether or not cough suppression remedies work is a question that preoccupies Ron Eccles and his colleagues at the Common Cold Centre (CCC), a clinical research organisation based at the University of Cardiff. Much of the work of the CCC involves testing remedies for companies including Pfizer, GSK, Boots Healthcare International, Bayer and Procter & Gamble. One recent study by the group showed that cough medicines with active ingredients such as codeine (2) and dextromethorphan are only 10-15 per cent more efficient than a placebo in reducing cough frequency.
The team also tested a single 30mg hard gelatine capsule of dextromethorphan compared with placebo by measuring how much sound the sufferer produces when coughing. ’Between 0 and 90 minutes we could show a significant difference between dextromethorphan and placebo, but over the whole test period there’s no real difference’, points out Eccles. ’Again, if you look at cough frequency the results are much the same. There is a small effect with dextromethorphan above placebo. But is it worth taking a medication to get that difference?’
According to Eccles the so-called ’powerful placebo effect’ can play a large part in many cough remedies - so much so that in some cases the syrup containing the active ingredient can be as helpful as the active ingredient itself. Eccles and his colleagues have also studied how codeine affects coughing using a 30mg dose in syrup. When they measured cough frequency with codeine versus placebo they found no great difference between the two. These and other results convinced Eccles that there is a large placebo effect with cough suppression. As a result of these cough trials Eccles’ concludes that hot honey and lemon or hot and tasty drinks could be some of the best treatments for a tickly cough because of their placebo effect. ’Anything that promotes salivation - be it acid or tasty, like honey and lemon, sweet and sour or spicy - will promote mucus secretion in the airway, and mucus has a soothing and beneficial effect. Mucus also traps viruses and bacteria - so it is our first line of defence against infection.’
Hot and spicy
Eccles also recommends a hot spicy curry to ensure that you salivate and reduce your coughing symptoms. ’Many spices have antibiotic or antiviral effects, particularly garlic and pepper, which could also be beneficial. There are also lots of natural remedies. How effective they are in placebo-controlled trials is debatable. But there is a lot of folklore and traditional medicine backing them up.’
However, Eccles is not dismissing the beneficial effects of active ingredients such as dextromethorphan and codeine in cough medicines. ’For dextromethorphan and codeine in the OTC doses we’ve got at present I’m not convinced that they are very efficacious. But they may be effective enough to give a 10 per cent or 15 per cent better than placebo response.’
The debate surrounding the efficacy of OTC cough remedies stepped up a gear last year with the publication in the British Medical Journal (2002, 324, 1) of a systematic review - or meta-analysis - by Knut Schroeder and Tom Fahey from Bristol University. Their study was a systematic review of the results of randomised controlled trials of OTC cough medicines for acute cough in adults. The researchers analysed the results of 15 trials involving 2166 people on cough remedies that contained active substances including antitussives, expectorants, mucolytics and antihistamines. The researchers stressed the need for caution in interpreting their results because of the relatively small number of trials in each drug category. However, they concluded that they couldn’t recommend OTC medicines because there was no good evidence for their effectiveness.
Not surprisingly, David Hull of P&G disagrees. In his opinion: ’A significant flaw in the Schroeder analysis is the inclusion of several studies of drugs not indicated as antitussives (cough suppressors), such as second generation antihistamines, mucolytics and expectorants. Inclusion of these studies in the meta-analysis dilute out the effects of studies that show benefits from true antitussive medication designed to treat cough’. Hull also recalls the meta-analysis of Lucy Pavesi et al that was not included in the review. This study published in Chest (2001, 120, 1121) determined that a 30mg dose of dextromethorphan delivers a 12-17 per cent reduction in cough sound over and above that of a matched placebo.
Ron Eccles also disagrees with the general findings of the Schroeder study. ’I think that anybody who goes to buy a cough medicine would benefit from it. But they are not getting the benefit from the active ingredient; rather they are getting the benefit from the soothing action of the syrupy vehicle and any cooling or warming compounds included in the mixture. While OTC cough medicines are effective, they’re probably not much more effective than a very good placebo. But if you want to pay money to buy a placebo then I don’t see anything ethically wrong with that.’
Clearing blockages
Relieving the more ’sticky’ problem of congestion or a blocked nose requires a different treatment. Topical decongestants, eg nasal sprays, contain compounds such as oxymetazoline and xylometazoline. These mimic neurotransmitters such as adrenaline or noradrenaline that activate receptors in the sympathetic nervous system, which controls, among other things, blood vessel constriction. ’The main cause of congestion in the nose is swollen veins or blood vessels which swell up and block the nose - not secretion or mucus’, explains Eccles. ’You can blow your nose but it will still be blocked. But if you constrict the blood vessels or veins you can open up the nose.’ Oxymetazoline and xylometazoline are effective blood vessel constrictors, often with efficacy for eight to 10 hours, which makes them effective night-time remedies. However, decongestants shouldn’t be taken for too long because of possible ’rebound congestion’ when the decongestant treatment causes the mucous membrane to swell. Note, however, Eccles says, ’this effect could be more related to the preservatives in the decongestant, which may act as irritants over a period of time, rather than the medication itself’.
Oral decongestants including ephedrine, pseudoephedrine and phenylephrine are not as effective as topical treatments because they bathe all the blood vessels in the body. ’This can give rise to side effects including hypertension or effects relating to the heart and blood vessel’, says Eccles. ’Because of these side effects, the doses are limited which leads to borderline effectiveness. I think that if you could increase the doses that these are available in, then you would get greater effectiveness, but would get more problematical side effects.’ However, explains Eccles, pseudoephedrine and ephedrine are popular treatments for sinusitis because they treat the whole of the nose and the sinuses compared with topical decongestants that are unable to get into and around the sinuses.
Other popular cold remedies for headache, sore throat and so on contain analgesics. Aspirin, paracetamol, ibuprofen etc, are usually very effective at reducing pain related cold symptoms. In general the inflammation associated with the common cold generates prostaglandins and the peptide bradykinin. These stimulate pain nerve endings, which produce sore throat, headache, muscle aches and pains, feverishness and sinus pains.
But what about the more ’natural’ components of cold remedies? Eccles is a great believer in menthol. Although it doesn’t actually decongest, menthol stimulates sensory nerves in the nose, which produces a feeling of decongestion. Also, by stimulating these nerves in the nose menthol can alter breathing patterns and therefore could be beneficial to infants, for example as a night-time remedy. Menthol is also a local anaesthetic, which is why it is used widely in sore throat lozenges. It also has antitussive properties so it makes for a good ingredient in cough medicine. More recently, menthol has been shown to be efficacious as a topical application, rather like an aromatherapy for headache.
Other ’natural’ remedies, however, have not so far convinced Eccles of their efficacy. ’We’ve done lots of work over the years on natural remedies, but none of it has ever been published’. For example, zinc supplements are controversial. Eccles’ view is that zinc is a vital nutrient for the immune system, and if you are short of zinc you will be at greater risk of infection. But it is i ts high dose use in lozenges that has proved controversial. As Eccles points out, some studies involving patients taking a 20mg zinc tablet every two hours, have shown that mega-doses of zinc work to help reduce the symptoms and duration of the common cold, while others have shown that zinc has no effect.
Flower power...
Another controversial remedy is Echinacea. Also known as the purple coneflower, Echinacea is a flowering plant indigenous to the US. Nowadays many people use it as a topical treatment for wounds, burns and insect stings and bites. While others, perhaps more controversially, believe that it stimulates the immune system and take it as a way to fight off colds and infections. Each of the nine species of Echinacea contains varying amounts of active ingredients, as do the particular parts of the plant. Typically Echinacea species contain polysaccharides, alkylamides, glycosides and alkaloids. However, whether any of these chemicals has an immunostimulatory effect is debatable. As Eccles explains, ’I believe that there is a growing body of evidence that shows Echinacea does influence the immune system and it may influence it in a beneficial way for infection’. The problem, Eccles says, is that there are so many different types of Echinacea product available. It is available as an alcohol extract or a water extract and can be extracted from the flower, root or the whole plant. It is very difficult to know exactly how much extract is present in the substances that you take.
Above all, says Eccles, there are problems with testing the efficacy of OTC or ’natural’ cold remedies: ’If you didn’t get a cold this year would you have got a cold if you had taken the remedy or not? Also, colds usually go away whether you medicate or not - so how long would it have taken without medication? And, lastly, how big is the placebo effect?’
Source: Chemistry in Britain






No comments yet