Paper's ubiquity and cheapness make it uniquely suitable for creating low-cost medical and environmental diagnostic devices. Rajendrani Mukhopadhyay investigates
Paper’s ubiquity and cheapness make it uniquely suitable for creating low-cost medical and environmental diagnostic devices. Rajendrani Mukhopadhyay investigates
A child dies from malaria every 45 seconds in Africa, equating to nearly 1 million infant deaths per year. Malaria is both a preventable and curable disease, but treatment needs to be started quickly once symptoms appear. And diagnosing it in remote clinics is currently reduced to an educated guess by healthcare workers with no access to diagnostic tools.
But what if clinic staff had a box of simple test kits, capable of giving an accurate diagnosis within a matter of minutes, and that were so easy to use that no technical skills or laboratory infrastructure were needed to handle them?

This is the goal of investigators developing diagnostic devices that can be printed on to sheets of paper. The tests are being designed to cost just pennies to manufacture - opening up the possibility of a plethora of diagnostic tests for tackling problems such as tuberculosis, cholera, environmental toxins and foodborne pathogens, which can be prohibitively expensive to diagnose in the developing world using other technologies.
Several organisations have been established around the world to develop and commercialise cheap paper-based diagnostic tests. US-based Diagnostics For All (DFA) was set up to turn the academic proof-of-concept devices coming out of the laboratory of George Whitesides at Harvard University, Cambridge, into large-scale manufactured commodities. The Canadian government sponsors the Sentinel Bioactive Paper Network, which consists of 24 academic research groups that focus on new diagnostic products made of paper. Thirdly, there is the Bioresource Processing Research Institute of Australia (Biopria), a part of the Australian Pulp and Paper Institute at Monash University.
Global commodity
Paper-like analytical products have been in the laboratory since the 19th century in the forms of filtration, chromatographic supports and litmus paper. These products tend to be made from purified cellulose or modified forms of cellulose - like nitrocellulose - rather than regular paper. ’Nitrocellulose is a speciality material produced in small quantities,’ states Robert Pelton of McMaster University, Ontario, Canada, who heads the Sentinel network. It is also extremely flammable, limiting its usefulness.
The new technology is instead aiming to use ordinary paper - the paper we use in bulk in our daily lives - as it is readily available worldwide. ’Paper is the cheapest, most ubiquitous material you can find,’ says Una Ryan, chief executive of DFA. ’In any city of the world, you can find comic books,’ she adds.

Ordinary paper consists of cellulose fibres combined with colloidal filler particles and soluble polymers. The ratio between these components is tweaked to produce papers with different porosity and surface properties (just think of cardboard compared to toilet paper). ’Paper is not a single substrate. It’s many different substrates, depending on what fillers and additives you use. You have a lot of control over porosity, surface charge, hydrophobicity and polarity,’ says John Brennan of Canada’s McMaster University whose laboratory is part of the Sentinel network. ’Paper as a platform has got as much versatility as any plastic that you could come up with, in terms of the kinds of surface chemistries you can use.’
Paper can be produced in large quantities at high speeds, with modern machines able to churn out 10m wide continuous sheets of paper at 100km/h. ’The efficiency is tremendous,’ exclaims Gil Garnier, director of Biopria. Because of the speed and efficiency of printing on paper, scaling up production of these devices would not be an issue, he claims.
Simply print.

Regular inkjet printers, the type many of us have in our offices, are used to produce the devices. First, a pattern of channels and reservoirs are designed with a computer program. Next, the printer’s normal ink cartridge is replaced with a cartridge containing a hydrophobic ink or wax. The computer design is then simply printed on paper.
Wax is restricted to the surface facing the inkjet cartridge, meaning an additional simple step is needed. The paper is placed on a hot plate to melt the wax, so it soaks through the paper. The result is a piece of paper with a pattern printed out in a hydrophobic wax that establishes the channels and reservoirs in three dimensions. ’This process takes about two seconds and costs 0.029 of a US cent - 1/300th of a penny,’ says Ryan. ’People can’t believe it when we tell them.’
The reagents for the biological or chemical assay can also be deposited using inkjet printing. Just the way a colour printer deposits different coloured inks in different locations on paper, a printer is instructed to deposit various reagents into the reservoirs. Alternatively the reagents can be combined with a sol-gel material, printed as a solution and then set into a gel to immobilise the reagents on the page. A number of devices can be printed onto a regular-sized piece of paper, then cut up into individual sensors.
.and test
To do the test, the device is dipped into a sample - be it blood, urine, soil extract or river water. The paper’s inherent porosity wicks up the fluid while the hydrophobic walls of the device guide the fluid to the various reservoirs. At the reservoirs, the sample reacts with the embedded reagents to generate coloured products.

So far, researchers have focused on enzymatic or chemical colour-change reactions, but alternative sensors are also being considered, such as using gold nanoparticles. Not all the important analytes will be present in sufficiently large quantities for easy colour change detection, so ’you will have to attach an enzyme, like horseradish peroxidase, or gold nanoparticles and multiply the signal’, explains Garnier.
According to Pelton, Sentinel network researchers were initially worried that using advanced technological entities, such as gold nanoparticles, would increase the cost of the paper test and void its primary advantage of cheapness. However, ’if you have a good sensor, it just doesn’t take very much material per test,’ he says. ’We don’t think cost is a limitation.’
Because paper is a complex mixture that contains a host of various compounds, they were also concerned that the paper components may interfere with sensing reactions. But after a series of experiments, Pelton is reassured. ’Our results suggest that standard biodetection agents aren’t too affected by paper chemistry’,
he says.
Looks good on paper
DFA is focusing on a device that tracks liver function, a prototype of which was earlier developed by the Whitesides group. A number of drugs, particularly for Aids and tuberculosis, are toxic to the liver and can prove to be lethal. ’In 25 per cent of cases in the developing world, the drug is going to cause liver damage,’ states Ryan. ’That number is only 2 per cent in the developed world, where patients are tested for liver function.’
The test consists of several assays for enzymes in blood to reflect the liver’s condition. It can survey the effects of drugs and even the progress of liver diseases, such as hepatitis C. ’If we can get this test to work, it solves a real problem in the developing world,’ says Whitesides. ’More critically, it will give us an end-to-end validation that the basic premise works.’
Meanwhile, Garnier and colleagues have developed a test for instantaneous blood typing that exploits blood flow on paper (See Chemistry World, June 2010, p4).1 Fresh blood wicks readily on paper. ’However, if you put some antibodies on the paper that are specific to the blood, it will agglutinate,’ explains Garnier. ’We discovered that agglutinated blood doesn’t wick at all.’
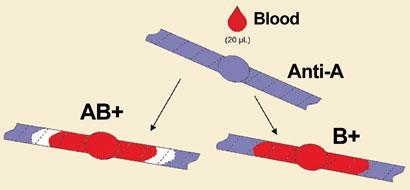
In the test, when red blood cells come into contact with antibodies embedded in the paper that recognise their particular proteins, the blood clumps and doesn’t flow through the channels. The test is able to distinguish between A+, B+, AB+ and O+ blood types. According to Garnier, the test will be critical in clinical settings for quickly assessing a person’s blood type.
Outside of the clinic
The food industry is another sector that may benefit from this research. A tiny embedded paper test could be included in food packaging to inform consumers if the perishable food within the wrapper is still safe to eat.
Teams at the Sentinel network have developed a test using DNA aptamers (single strands of DNA that specifically bind to target molecules) attached to gold nanoparticles.2 When the strip comes into contact with a specific food pathogen, it turns an intense red colour within minutes. ’As pervasive as printed barcode labels are on consumer goods, foods and everything else, we think it’s possible to ultimately have an appropriate toxin or pathogen detection label printed right beside the barcode,’ envisions Pelton.
For environmental analyses, Brennan’s team has developed a paper-based colorimetric sensor to detect organophosphate pesticides, which are still illegally used in some parts of the developing world to spray agricultural crops.3 The sensor detects nanomolar quantities of pesticides within five minutes in foods like milk and lettuce. ’This pesticide strip has probably now generated over 200 requests worldwide from people who want to buy, manufacture or distribute it,’ says Brennan. ’We’ve clearly hit a nerve.’
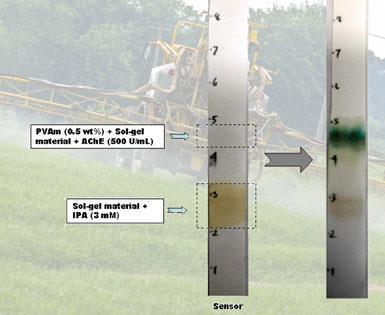
Dial-a-diagnostic
Creating an assay is only one aspect of diagnostics, however. Equally important is what happens with the information generated: how will the data be analysed and by whom?
Ideally, the test will provide a yes or no answer - much like a home pregnancy test - which a user with no technical training can interpret. However, not all tests provide yes or no answers. Semiquantitative tests measure the amount of a certain analyte, which dictates the type of treatment necessary. These devices have to be read by someone skilled in the art of data interpretation. But how can that be done in places like sub-Saharan Africa, where technical specialists are rare and may be located miles away?
Modern technology comes to the rescue. ’I think we’ve established that the old system of transmitting information over the phone and relying on someone to record it with pen and paper probably hasn’t been successful in a lot of places in the world,’ says Roger Peck, a research scientist interested in implementing rapid, affordable diagnostics in the developing world at the charitable organisation Program for Appropriate Technology in Health (Path). ’There is great hope with cell phone cameras and cell phone networks.’
Most modern mobile phones come with a built in camera and email capabilities. So once a colour-change test has been completed ’you can snap a photograph and email it to your doctor’, says Ryan,4 who will then read the result for you.
Because of their low cost, paper tests can be administered repeatedly and photos can be emailed to centralised databases. Thanks to a cell phone’s inbuilt global positioning system (GPS), photographs can even be tagged with a location. Peck and Ryan imagine public health organisations using paper diagnostics combined with telecommunications to track vitamin A deficiency in a population or the spread of an influenza strain around the globe.
There are, however, obstacles to getting the data over phone networks. For one, photograph quality isn’t uniformly consistent, owing to differences in phone and user abilities. DFA is currently working with some telecommunications companies to correct for such photographical errors. They are developing algorithms that will correct for brightness, intensity and angle in a photograph. Pictures of the tests could also be taken alongside colour calibration strips, so that the analyte amounts in the tests may be correctly assessed.
Making it happen
Garnier, Brennan and Pelton all hope to have paper tests appearing on the market within the next two to five years, but there are still hurdles to overcome. Technical details that still have to be nailed down include understanding which types of paper work best for which applications, and how to immobilise more delicate enzymes on paper without denaturing them.
Then there are the logistics of distribution. Here, economics comes into play. To provide motivation for investment in the tests, someone has to be able to make a profit, however small, from manufacturing, distributing, and selling them. Path and DFA are considering several avenues - such as the Grameen Bank model, in which small loans are given to local people to enable them to start selling test kits. Using the profits from these sales they can slowly build up viable businesses, become financially independent and pay back the loans.
Another concern is how people in the developing world will react to the tests. ’Social acceptance is a critical issue,’ says Garnier. ’Should the test confront taboos, for example in India, it will simply not be used.’
But experts say it will be obvious when they’ve hit the right approach. ’Our success is going to be when we send 10,000 of these tests to India or Brazil and we get back a note saying, "they worked really well, please send us another 100,000 more",’ says Whitesides.
Rajendrani Mukhopadhyay is a science writer based in Washington, DC, US
References
1 M S Khan et al, Anal. Chem., 2010, 82, 4158 (DOI: 10.1021/ac100341n)
2 W Zhao et al, Anal. Chem., 2008, 80, 8431 (DOI: 10.1021/ac801008q)
3 S M Z Hossain et al, Anal. Chem., 2009, 81, 9055 (DOI: 10.1021/ac901714h)
4 A W Martinez et al, Anal. Chem., 2008, 80, 3699 (DOI: 10.1021/ac800112r)






No comments yet