The ability to wipe out traumatic memories is just around the corner. Katrina Megget looks into the science of forgetting
The ability to wipe out traumatic memories is just around the corner. Katrina Megget looks into the science of forgetting
There’s no time to think. A car is hurtling towards your vehicle at an impossible speed. Before you can blink, you find yourself hanging upside down held in place by your seatbelt. And ever since, you have been unable to set foot in a car.
But what if the fear associated with the car crash could just evaporate? What if you were no longer scared when you smelt burnt rubber or caught a whiff of petrol fumes?

It might sound like science fiction, but researchers are taking steps towards developing a drug that could do just that - erase the fear associated with traumatic events. And it’s not just the distressing memories experienced by people suffering post traumatic stress disorder (PTSD) that are being targeted - phobias and even addictions could benefit from this research.
Overcoming a fear of spiders
In February 2009, a landmark study was published in Nature Neuroscience , where human volunteers were cured of a fear response to spiders - by taking the beta blocker blood pressure drug propranolol. The study, carried out by a Dutch team at the University of Amsterdam, took advantage of a relatively new finding that memories could be manipulated when recalled.
In the experiment, human volunteers were shown the images of two different spiders - one was accompanied by a pain stimulus, while the other was not. The volunteers soon developed a fear response to the spider associated with pain. A day later this fear memory was recalled by viewing the image again, but just before this reactivation the volunteers took propranolol.

Previous studies had shown that taking propranolol as soon as a life-threatening event occurs can stop the traumatic memory being seared into the brain in the first place. The Dutch study took this forward to show that propranolol still has an affect some time after the event. Significantly, the ’cured’ volunteers remembered the association between the spider and the pain but were unable to remember the emotional response to it.
These results could be deemed a breakthrough in treating anxiety disorders such as PTSD. ’But we are still on the cusp with this research,’ explains Karim Nader, neuroscientist at Canada’s McGill University in Montreal. ’Some people have had PTSD for 30 years and in individual case studies of memory disruption the vast majority [have not experienced a return of symptoms] even after 6 months. That’s crazy right? There’s currently no 100 per cent guarantee treatment for PTSD, that’s why we should go for it.’
Using propranolol to disrupt memories draws on research by Nader that had turned the traditional theory of memory on its head. In the past, it was thought initially unstable memories became consolidated and wired into the brain and that was it - they were fixed and could not be tampered with. But what Nader discovered is that every time the memory is recalled it becomes unstable again, before being reconsolidated.
The best guess is that there are specific proteins, such as receptors, that increase or decrease the talking between neurones in memory storage, he says. During normal reconsolidation these proteins degrade and are replaced, but if the cell can’t replace the proteins then memory storage is disrupted. It is this window of instability during recall - a mere few hours - that could potentially provide a way of treating PTSD, phobias and drug addictions. Nader says if pharmaceuticals can be introduced that hinder memory restorage then patients could be cured.
Tackling PTSD
The memories associated with PTSD are so strong that the brain mechanics are ’blown away’ and there is no longer any control on the memory, Nader explains. Current treatments - cognitive behavioural therapy and eye movement desensitisation and reprocessing - are only about 60-80 per cent effective but results can vary greatly, and for many PTSD sufferers will never be a solution.
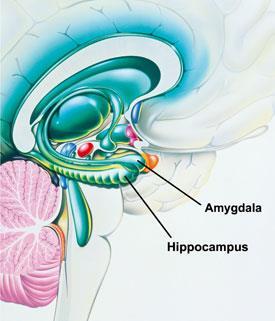
The idea behind memory disruption, says Nader, is to target just the emotional memory, which is located deep in the brain in the amygdala. That way the conscious memory of the event - located in the hippocampus - remains intact and remembered, while the emotional part associated with the event is weakened and effectively forgotten. This is how propranolol seems to work. Through propranolol receptors in the amygdala, the drug blocks the action of adrenaline, a stress hormone that strengthens emotional memories.
’If we can block the memory even by 50 per cent then it’s just at a level of a manageable bad memory, so it becomes responsive to current treatment,’ Nader says. And when PTSD affects 4-5 per cent of British soldiers and up to 30 per cent of road accident victims, military psychiatry expert Neil Greenberg, from King’s College London, UK, predicts that PTSD patients would be interested in such a drug. ’Conceptually’, he says, ’it’s a nice idea if you can break down the unhelpful emotional memories associated with the event’.
Medicines under investigation
Greenberg questions whether propranolol is the best vehicle to meet this aim, but for Nader the beta blocker is his favourite option right now, though there are many other chemicals being investigated, some already approved by the US Food and Drug Administration for treating other illnesses.
One such molecule is the stress hormone corticosterone. According to research at UT Southwestern Medical Center in Texas, mice that were injected with corticosterone when the trauma of an electric shock was recalled showed a lower fear response when later exposed to the same environmental cue. The belief is that corticosterone stimulates a new memory during recall, thereby weakening the original traumatic memory. But how exactly this works is not clear, explains lead researcher Craig Powell. ’At this point, we don’t fully understand the mechanisms by which corticosterone is acting. But this is an area of active investigation and that in itself may lead to additional novel downstream targets for drug discovery.’ And with stress hormones seemingly playing an important role in traumatic memory development - possibly in order to give an evolutionary survival edge - the possibility of various targets could be endless.
For example, animal research published in 2009 looked at another stress hormone cortisol and how it was blocked by the abortion drug RU38486. Scientists at the Mount Sinai School of Medicine, New York, US, found that administering RU38486 in rats shortly before or just after recalling the memory selectively reduced the stress-related memory. The research also showed that the effect was long lasting. Cristina Alberini, a neuroscientist on the Mount Sinai team, believes their research suggests the abortion drug is a potential novel target for PTSD, adding it might even have one up on propranolol. ’In our [tests] propranolol does not disrupt reconsolidation [in rats] whereas RU38486 does it very effectively. More studies need to be done, though, in order to understand what RU38486 or propranolol disrupts and whether one is more efficacious than the other.’ Likewise, clinical studies will need to be designed to investigate the effect on human memory reconsolidation, she says.
However, reconsolidation is not the sole line of enquiry in research to cure fear memories. Much work has been done on a method called drug-free extinction training, where conditioned fear responses can be extinguished by repeatedly exposing a patient to the environmental cue they previously associated with fear or pain, without the pain stimulus present. The fear response is not erased but instead replaced by a new ’safe’ memory.
Now, a team at the University of Puerto Rico school of medicine, with support from the US National Institute of Mental Health, has found a naturally occurring brain protein - brain-derived neurotrophic factor (BDNF) - can be used as a substitute for time-intensive extinction training by inducing the creation of safe memories. In the 4 June issue of Science , the researchers reported a study on rats conditioned to fear a tone of voice by association with an electric shock to the foot. The animals that had BDNF infused into the infralimbic prefrontal cortex brain region no longer froze in anticipation of the electric shock when exposed to the tone - the same effect as if they had received extinction training. Meanwhile, other research has shown that rats deficient in naturally occurring BDNF are more likely to do poorly in extinction trials.
Beating addictions
But it’s not just post traumatic stress disorder that scientists are hoping to help us forget. Memory disruption in drug addiction has also had some success, as Jonathan Lee from the University of Birmingham, UK, has found. This is because the amygdala also plays an important emotional role in addictive drug-related behaviour - a stimulus that elicits a memory of drug-taking, such as a syringe or specific people, is often the reason behind a relapse. Initial research by Lee’s team in rats highlighted a specific gene in the amygdala that, when inactivated, selectively impaired these memories. Additional research has since found that when just prior to memory recall, a patient is given a chemical that blocks the action of the NMDA-type glutamate receptor, which has a role in learning and memory, drug-seeking behaviour is reduced.
Meanwhile, University of California, Irvine, scientists have been looking at cocaine-associated memories in the nucleus accumbens, an area of the brain that receives neural input from the amygdala and is involved in motivating reward-seeking behaviour. Training rats to associate one of two chambers with cocaine, the researchers found that chemicals - such as U0126 - that blocked the extracellular signal-regulated kinase regulatory pathway prevented the animals’ memory retrieval of their preference for the cocaine chamber. While more preclinical work needs to be done before these studies can progress onto humans, Lee says with the success of propranolol ’the potential for a therapeutic is very real’.
However, with the discovery of the malleable memory comes the concern that memory disruption via drugs might affect other memories. Nader and colleagues looked into this in rats and found this was not the case - only directly reactivated memories are vulnerable to disruption; associated ones are not affected. ’In the work in animals it seems that only the trauma memory would be affected and that others don’t undergo reconsolidation,’ Nader says, but he admits they currently can’t tell if other memories are reactivated in the recall process. By the same token, Lee says more than one memory might need to be disrupted in order to treat the disorder, especially if memory recall involves various stimuli. ’If an important stimulus is omitted, that stimulus may remain capable of triggering anxiety even after the treatment. This question of the generality of the effect is only beginning to be addressed experimentally in preclinical research.’
Wiping the slate clean
There is one drug, however, that is known to affect other memories - indeed, it completely wipes them all out. This research carried out by neuroscientist Todd Sacktor, from the SUNY Downstate Medical Centre, New York, US, has gone some way into understanding the intricacies of the mechanism of memory storage and potential drug targets.
The main outcome of Sacktor’s research is the discovery of the protein kinase Mzeta (PKMzeta ), which appears to be the molecule that sustains long-term memory storage. It seems to work as a conveyor belt to somehow continuously push neurotransmitter receptors into the synapse. In 2006, Sacktor showed that all memories in the hippocampus can be erased by an investigational drug - a pseudosubstrate inhibitor called zeta inhibitory peptide (ZIP) - and this happened regardless of whether memories were recalled or not. ZIP was found to bind to PKMzeta , blocking its phosphorylating action and possibly causing the molecule to drift away from the synapse. The memory wipe-out action of ZIP appears to be permanent, Sacktor says, but it only affects the brain regions it is injected into and it doesn’t stop the formation of new memories in the future. ’It’s not damaging the brain, it’s just erasing the memory already there,’ he says. ’Once ZIP wears off you can store new memories.’

The whole process still needs unbundling, which Sacktor is working on. ’We would have to come up with other tricks to make it more like reconsolidation. It’s too powerful to use on people,’ he says. ’And how to make it specific to wipe out individual and not all memories in a brain is something we don’t know how to do yet.’
Ethical issues
While the therapeutic possibilities of all this memory disrupting research are exciting, it does bring up some unsettling ethical questions. Is it a slippery slope? Where do you draw the line at which memories can be disrupted? What about the implications for legal cases? How does this affect our personal identity? Indeed, is altering memories even an appropriate medical intervention?
’It’s not so much whether it’s appropriate or not,’ says Nader. ’It’s being used as a way of altering psychopathologies and given the way we are doing it - preserving the conscious part and bringing the emotional part down to a level that will be responsive to treatment - is not compromising the effect of the conscious memory. All it is is fixing a memory so big the brain can’t deal with it. It’s not an ethical issue. This can give people back their normal lives.’ Indeed, Nader says evidence from the PTSD patients who used propranolol suggests they are not perplexed by the memory disruption for this very reason - they now feel they can move on with their lives.
This is echoed by Lee: ’a patient with PTSD is partially defined by their condition - it is part of their identity, but a part that is debilitating. So the goal of treatment could be viewed as returning the patient’s identity back to "normal".’ Bioethicist Ruud ter Meulen, director of the centre for ethics in medicine at the University of Bristol, UK, agrees: ’if propranolol or new drugs are helping people to better cope with stressful events I cannot see any reason why this would be unethical. Actually, on the contrary, it would be unethical not to treat people with these drugs. And if I was in such a situation I would certainly consider the use of such a drug if appropriately supervised by a competent doctor.’
Sacktor says that if any ethical questions should be raised by the research, then they are more likely to apply to memory enhancers than disruptors. ’People generally don’t want to erase their memories unless they have PTSD, but people will want to enhance their memory. That’s going to bring some big ethical issues.’ Regardless though, memory disruption is like any technology, he says. ’Take fire. Fire is a good thing to cook meals and keep us warm but if a pyromaniac uses it then it’s not so good. It’s true for any technology. This is just a powerful one because it affects the human sense of self, which is based on our memory.’
This research might have thrown up many questions, but it has opened up a world of possible treatments that previously had only been dreamed about. Baby steps, yes. But this is just the beginning along the road that is the science of forgetting.
Katrina Megget is a freelance science writer based in London, UK






No comments yet