Anthony King examines a crucial part of vaccines that can significantly boost their performance, but which often go unrecognised
Vaccines prevent millions of deaths and illnesses every year, yet an essential component of them is often overlooked – adjuvants. These press the immune system to take appropriate action against the accompanying live or weakened invader in the vaccine. Right now, much vaccine effort is focusing on the novel coronavirus (Sars-CoV-2, causing the respiratory disease Covid-19), and choosing the right adjuvant may be crucial (see box below).
It will not be easy. Experts say the low-hanging fruit in vaccine development are gone. Pathogens with no vaccines are complex, challenging organisms, and require new sophisticated help from adjuvants. Progress has been made, as exemplified by blockbuster shingles vaccine Shingrix released in 2017 and malaria vaccine Mosquirix rolled out in 2019, both underpinned by adjuvants.
‘Adjuvants have really taken off in the last 10 to 15 years,’ says John Tregoning, a virologist at Imperial College London in the UK. ‘They have a qualitative and quantitative effect – some increase the total immune response, some change the shape of the immune response.’ Adjuvants though have a surprisingly long – if lonesome – history. The very first were aluminium salts (alum), introduced into human vaccines in 1932. These appeared as contaminants in aluminium vessels, but serendipitously boosted immune responses. ‘When they started making vaccines in a really clean way, the effects often disappeared,’ says Mark Coles, immunologist at the University of Oxford in the UK.
Alum would be hard to get licensed nowadays
Remarkably, alum was the only adjuvant licensed in human vaccines for around 70 years. It stimulates antibody production and is in around 30 vaccines today, including those against hepatitis B, polio and pneumococcus. But we still don’t know precisely how alum works.
‘Alum would be hard to get licensed nowadays,’ says Wolfgang Leitner, who leads the adjuvant research programmre at the US National Institutes of Health in Maryland. ‘But it is easy to get into vaccines now given the gigantic safety database.’ Approximately 3 billion doses of alum have been administered in vaccines. ‘The long safety record is one reason alum was the sole adjuvant for so long. The other was the slow progress in our understanding of how disease protection is initiated,’ says George Mutwiri, a vaccine scientist at the University of Saskatchewan, Canada.
Alum was not required, however, in live viral vaccines such as those against measles, mumps or rubella. These infections look concerning enough for the immune system to kick into gear. ‘In the past you took a pathogen, inactivated or attenuated it, and you have the antigen and the adjuvant as part of that killed or attenuated pathogen,’ says Leitner. Today’s vaccines often rely on recombinant proteins made in bulk in cell systems. ‘Modern vaccinology is focused on synthetic vaccines where scientists identify a specific portion of the pathogen that generates an immune response,’ explains Chris Fox, who led adjuvant formulation at the recently closed Infectious Disease Research Institute in Seattle, US.
Adjuvants trick your body into thinking there is an infection
These synthetic fragments need a helping hand. ‘We now have to reconstitute what is in a natural, old-style vaccine, but in a more controlled and deliberate fashion, where we take parts of the pathogen and some immune-stimulators,’ says Leitner. As Coles puts it: ‘Adjuvants trick your body into thinking there is an infection and activate the right cells.’ Tell-tale molecules on bacteria or viruses put invaders in the crosshairs. ‘Nature has a system for identifying foreign entities. Adjuvants are meant to mimic that system,’ says Nathalie Garcon, chief executive of the Bioaster research institute in Lyon, France.
The purity of vaccine antigens made via genetic engineering has downsides, exemplified in the vaccine for pertussis, or whooping cough. A pertussis vaccine was first developed in the 1920s, and for decades a whole-cell vaccine proved extremely effective. However, many people receiving it experienced side effects, such as swelling or fever. It was largely replaced in high income countries with a safer protein-based pertussis vaccine formulated with alum, first made in the 1990s.
Alum increases an antibody response that targets extracellular agents (a type 2 immune response, TH2), crucial for say tetanus and polio, but it is not so good at inducing a cellular immunity, mustering specialist T cells to fight bacteria and viruses inside cells (a TH1 response). The result is that the new vaccine prevents whooping cough, but does not stop a person becoming infected and passing on this contagious respiratory bacterium. ‘The acellular pertussis vaccine is not as protective, which is why we have outbreaks of whooping cough now,’ explains Tregoning. Its protection wanes more quickly too.
This is not to say newer vaccines are inferior. Using recombinant proteins simplifies and increases the scale of manufacturability of vaccine antigens, reducing costs while improving predictability. What the pertussis vaccine arguably requires is a better adjuvant, one which triggers a type of T helper cells (TH1s) that primes the body to take aim at foes residing within cells.
Treating the new coronavirus

Vaccines based on viral proteins are in focus for the novel coronavirus, Sars-CoV-2. ‘Anyone working with this protein-based vaccine will need a good adjuvant,’ notes Wolfgang Leitner, adjuvant programmer leader with the NIH. He says traditional alum is not an ideal adjuvant here, because it induces the wrong immune response – a TH-2 response led by antibodies.
‘Good TH-1-driving adjuvants will be in demand,’ Leitner explains. This includes those based on bacterial DNA sequences – CpG sequences, which stimulate TLR9 receptors of our frontline defenses, the innate immune system.
Leitner warns that two safety challenges face developers targeting the novel coronavirus. First is more severe illness because the vaccine primes the wrong type of immune response. This notoriously occurred in 1967 with an inactivated respiratory syncytial virus (RSV) vaccine that caused a non-protective immune response, which led to a more severe illness when the children later became infected by the wild virus.
The second problem happens when an antibody response against a first infection or vaccination fails to protect against the virus, but actually help it infect that person. Leitner is hopeful though that modern adjuvants will prove more predictable: ‘A lot of novel adjuvants trigger very specific, well understand cellular and molecular pathways.’ He is promoting side-by-side comparisons of adjuvants with the same vaccine candidate to figure out which is most protective. These are mostly from academics and small companies.
Unfortunately, some highly successful adjuvants from big pharma, such as GSK’s AS series, are unavailable to investigators. ‘Pharma companies that get a vaccine approved that contains a new adjuvant have really no incentive to make that adjuvant available for research by others,’ Leitner explains. If anyone produces problematic data with their adjuvant, this could affect the approval or sale of their product even if their product is fine. And problems could arise because they didn’t chose the wrong route or excessive dose or because it was a bad match for the vaccine, explains Leitner.
DNA and RNA vaccines being developed against Sars-CoV-2 do not require adjuvants. These act more like a virus, igniting an immune response geared towards wiping out infected cells.
Hard to get
Researchers tried to develop HIV and malaria vaccines in the 1980s, but one barrier was that alum did not stimulate enough of a cellular immune response. The search was on for new immune modulators. Important new adjuvants were discovered around this time: a detoxified version of a salmonella toxin, mono-phospholipid A (MPL); the detergent-like molecule QS21; and specific CpG sequences of bacterial DNA. GSK led the way in mixing alum with these new adjuvants and systematically testing their effectiveness.
The approval of AS04 was a huge breakthrough
In 2009 the US Food and Drug Adminstration for the first time approved a vaccine with an adjuvant that was not alum – a combination of MPL adsorbed onto aluminium hydroxide or aluminium phosphate, termed AS04 by GSK. ‘That was a huge breakthrough,’ says Leitner. A significant help had been the discovery in the 1990s of toll-like receptors (TLRs), which help switch on the innate immune system. MPL was found to latch onto TLR-4, which triggers a response against viral infections (the so-called TH1-biased response). MPL originated in the 1970s, when a Montana-based biotech modified an endotoxin (lipopolysaccharide), showing the slow pace that vaccine development can have.
AS04 became a critical part of Ceravix, GSK’s vaccine against human papilloma virus (HPV), approved in 2009. The combination adjuvant induced immune memory cells, giving long lasting protection. Ceravix targeted cancer-causing HPV strains 16 and 18, but covers other HPV strains too, because of the adjuvant, says Garcon. The original endotoxin from Salmonella was modified by chemists to make MPL less reactogenic, while triggering a potent enough immune response, and minimising inflammation.
Carefully formulated liposomes – a spherical vesicle with a geometry and size similar to a virus – is another strategy of adjuvant developers. ‘Formulation is more important in adjuvants than for other pharma products, because you want to target and activate the appropriate cells,’ says Fox. Tailoring the response is especially crucial against complex pathogens that lie latent, like tuberculosis, or which switch between life stages, such malaria, but this is a formidable hurdle. ‘We haven’t seen good vaccines against parasitic diseases yet,’ notes Fox.
A mediocre vaccine was significantly improved by adding the right adjuvant
This is despite huge amounts of effort and money directed towards a vaccine against the malaria parasite, Plasmodium falciparum. After almost three decades, GSK last year began rolling out its Mosquirix vaccine in three African countries, to immunise at least 360,000 children a year until 2022. It has not received market approval yet, and there are some concerns around its safety and durability. A critical component of this breakthrough RTS,S vaccine (Mosquirix), however, is an adjuvant developed by GSK – AS01. ‘This was a mediocre vaccine, but was significantly improved by adding the right adjuvant,’ says Leitner.
For Mosquirix, GSK’s AS01 combined MPL and QS-21 in liposomes. QS-21 is an unusual ingredient: an acetylated saponin from the bark of a South American soap tree, Quillaja saponaria, first used in veterinary vaccines. QS-21 combined with MPL provokes an antibody and a T-cell response. The value of the AS01 adjuvant is clear from the vaccine against shingles. This painful disease occurs as people age or become immune-suppressed, because when T-cell memory drops, the chicken pox virus (Varicella zoster) reactivates. The Shingrix vaccine from GSK contains AS01 and was approved in 2017; it is over 90%.
An alternative vaccine, Zostavax, is based on an attenuated virus and the dose given to the elderly is 10 times that given to children for chickenpox. ‘You would think that would be the best way to stimulate an immune response,’ says Garcon. It reduces the risk of shingles by 51% in 60–80 year olds, but over the age of 80 protection falls to 18%. The recombinant antigen plus AS01 adjuvant in Shingrix, however, offers 97% protection to 50–70 year olds, and more than 90% to those aged over 80. ‘Here is a case where an adjuvant is able to generate protection that even an attenuated pathogen cannot manage,’ says Garcon, who headed up GSK’s adjuvant R&D for many years. Shingrix, launched in 2017, was predicted to exceed £1 billion in sales in 2019.
For TB we are not much further on than we were in the 1880s
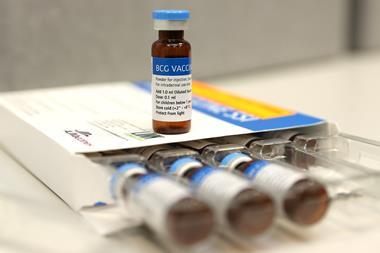
The AS01 adjuvant is also included in a GSK candidate tuberculosis vaccine, which was reported to protect against lung disease for at least three years. Each year around 10 million people become ill from TB, but the only licensed vaccine (BCG) has been around for nearly a century. It is made from a weakened strain of Mycobacterium bovis which is very effective in children but suboptimal in adults. ‘People are trying to make better TB and malaria vaccines, and there is a number of ongoing clinical trials,’ says Coles. ‘But for TB we are not much further on than we were in the 1880s.’ Fox says it is not yet clear what is required for an effective vaccine, but cellular immunity plays a big role in protecting against TB, ‘and hence we need new adjuvants’.
GSK’s TB vaccine with AS01 shows promise, but there are concerns. ‘There is a supply crunch on the shingles vaccine, which is a highly profitable vaccine,’ says Fox. ‘How in the world is there going to be enough supply of the same [AS01] adjuvant for vaccines like TB and malaria, where presumably the profit margins are much slimmer.’ A group at the Statens Serum Institut (SSI) in Denmark is also developing a TB vaccine, using IC-31 adjuvant from speciality vaccine company Valneva, consisting of a peptide and synthetic DNA.
The Danish group also developed its own ‘cation adjuvant formulation’ platform. This comprises a positively charged liposome and a synthetic analogue of a lipid from the tuberculosis membrane, with or without other immune stimulators. It seems likely that future adjuvants will continue to combine multiple ingredients. For example Mutwiri’s group has developed a triple combination adjuvant consisting of a polymer, sequences of DNA and peptides. The peptides call immune cells to the injection site, the DNA stimulates a strong TH1 antibody response and the polymer a TH2 cellular response.
Universal flu vaccine
The World Health Organisation estimates there are 3–5 million severe flu cases each year, with the elderly most at risk of death. But flu vaccines don’t work so well in the old, as our immune response declines with age. One way to compensate is to add adjuvants to boost the response. One vaccine developed for the elderly (Fluad) includes the adjuvant MF59, an oil-in-water based emulsion of squalene oil. An alternative is a high-dose vaccine containing four times the amount of antigen as regular flu vaccine.
Adjuvants allow you to get lots more doses out of your vaccine supply
Squalene, says Dennis Christensen, who leads adjuvant research at SSI, resembles signals of cell damage and attracts macrophages and other immune cells to the injection site. GSK also developed AS03, an emulsion-based adjuvant consisting of squalene and vitamin E, which induces a marked antibody response and is used for its pandemic flu vaccine, Pandemrix. A major challenge with pandemic flu outbreaks is that it will be impossible to make enough antigen, but adjuvants can ride to the rescue. ‘Adjuvants allow you to get away with a lot less antigen and get lots more doses out of your vaccine supply,’ says Leitner.
Some novel adjuvants seem to stimulate a better response to new flu strains, which may ultimately allow for a vaccine that protects against all newcomers. ‘One of the big priorities of our institute is to support the development of a true universal flu vaccine, one that is effective across multiple years,’ says Leitner. This requires an antigen design, with adjuvants, that directs the immune system to part of the virus that is highly conserved between strains in different years. The NIH is unusual among public funders in that it purposely funds adjuvant development and attracts praise from vaccine researchers.
Another adjuvant strategy is to provoke the body using nucleotides that look foreign. Sequences of unmethylated cytosine followed by guanine (CpG) are recognised as unusual by our immune system, picked up by antigen-presenting cells and then engage TLR9 within those cells. This in turn sets off a cascade of pro-inflammatory cytokines, which leads to antibody-secreting B cell and T cell response.
The US approved a hepatitis B vaccine in 2018 (Heplisav) that was the first one to use a short DNA sequence as an adjuvant. Developed by Dynavax Technologies, this vaccine offers a 95% rate of protection, superior to the existing vaccine Engerix-B, while requiring two rather than three shots. The synthetic CpG sequences proved to be potent stimulators of TLR9. The NIH has funded a group at Flinders University in Adelaide, Australia, that ran computer screening on DNA sequences to uncover those which mimic bacterial DNA, which is being tested in a flu vaccine. Leitner expects more vaccines to use oligonucleotide sequences, tailored so that they have different effects on different immune cells. ‘You can tweak the response by using different CpG sequences,’ says Leitner.
GSK dominance
It is impossible to overlook the dominance of GSK in adjuvant development. The company recognised the importance of adjuvants early. It acquired Corixa for $300 million in 2005, to access adjuvant MPL, which GSK was using in its vaccine pipeline. Garcon recalls that other companies took different paths. ‘Merck took the route of DNA vaccines; Sanofi went for live vaccines,’ she says. ‘That was because GSK was the first company to do a recombinant antigen vaccine, Hep B, and it was understood that it would need an adjuvant.’
Small companies find it difficult to develop, manufacture and distribute vaccines at scale. ‘Some adjuvants are developed by small entities and then are acquired by large companies such as GSK,’ says Leitner. The NIH aims to encourage a pipeline of adjuvants, because transitioning for the lab to clinic to market is an extremely slow process in vaccines, where acceptance for safety risks is almost nil.
Adjuvants are not products by themselves. They are approved as part of a vaccine. Nonetheless, GSK has showcased adjuvants as a platform technology, with one (ASO1) proving crucial in its blockbuster shingles vaccine, in its frontrunning malaria vaccine and a promising TB vaccine. Adjuvant development is now of interest to big pharma, and smaller biotech, which are trying to catch up with GSK. And as its blockbuster shingles vaccine has shown, advances in adjuvants can spur on the development of effective and extremely profitable new products.
Anthony King is a science writer based in Dublin, Ireland









No comments yet