Companies are convincing regulators, but will doctors use them, and will providers pay for them?
The makers of the Alzheimer’s disease antibody treatment Leqembi (lecanemab) have convinced regulators in the US to upgrade its status to full approval, based on further trial data received after the anti-amyloid antibody was granted accelerated approval in January.
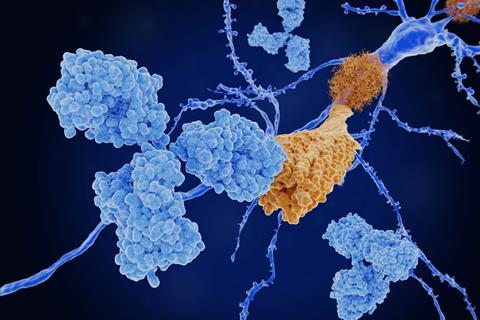
This means the drug may now be made available through the US’s national Medicare healthcare scheme, while other insurance providers will make their own judgements about whether and how they cover it.
Meanwhile, results from trials of Eli Lilly’s similar antibody, donanemab, have shown similar abilities to clear amyloid from patients’ brains, and slow their cognitive decline in the early stages of Alzheimer’s. The company will now apply for regulatory approval in the US.
These results are definitely encouraging. They confirm (after decades of failures) that pharmaceutical intervention can have a measurable effect on a massively debilitating disease. But it’s also worth keeping in perspective that these drugs provide a modest slowing of the disease’s (so-far) inevitable progress – by just a few months over the course of an 18 month trial. They are not cures, and cannot reverse any loss of cognitive ability.
They also come at relatively high cost, both financially and in terms of medical resources. They involve monthly intravenous infusions, and patients must be regularly monitored for side effects, including undergoing brain scans to check for swelling or bleeding.
Biogen and Eisai seem to have convinced the US Food and Drug Administration (FDA) that, in the absence of anything better, these antibodies are worth a try. The next few months and years will determine whether physicians and the holders of the purse strings agree that the benefits justify the administrative, financial and side-effect burden.
It will likewise be pivotal to see what regulators elsewhere around the world make of lecanemab and those antibodies that follow. The European Medicines Agency (EMA) was much more circumspect that its US counterpart when considering Biogen–Eisai’s first-generation Alzheimer’s antibody. While the FDA allowed Aduhelm (aducanumab) onto the US market in 2021 (admittedly with various restrictions under its accelerated approval pathway), the EMA rejected it for lack of sufficient benefit, and Biogen withdrew its application for approval. In the end, it has effectively failed to convince doctors and healthcare providers of its value.
The clinical trial data for lecanemab and donanemab are definitely stronger and more convincing than for aducanumab, but the clinical benefits remain modest and the side-effect threats remain. As ever, it comes down to the balance between benefit and risk.













No comments yet