With litigation against suppliers in full swing, how does the US counter its addiction to powerful painkillers?
Opioid drugs play an important role in treating acute pain, whether post-surgery or in the immediate aftermath of serious trauma. Morphine, its derivatives and various synthetic analogues also have a place in end-of-life care for cancer patients when their pain becomes overwhelming. But in the US there is now a growing crisis of addiction to opioid medications.
The figures are startling. The Department of Health and Human Services (HHS) claims opioid overdoses killed more than 47,000 people in the US in 2017 – almost 130 a day – and 36% of those involved prescription opioids. Two in three drug overdose deaths now involve opioids, and this has increased six-fold since 1999.
This is perhaps the biggest public health tragedy ever created through the deliberate actions of people. It took hold over the course of decades of action and inaction. It will, unfortunately, take years of aggressive action to reverse its course
Scott Gottlieb, FDA Commissioner
While the drugs give short-term relief from pain, patients develop tolerance and ever greater doses are required for the same effect. Many find their prescribers become reluctant to write further prescriptions, leaving them addicted and reliant on illegal suppliers, or even resorting to heroin.
Frighteningly, HHS says almost 80% of heroin users started out by misusing prescription opioids. And now the synthetic opioid fentanyl is making headlines, too. First made in 1960 by Paul Janssen, it is at least 50 times more potent than morphine, greatly exacerbating the potential for inadvertent overdose. Its synthesis is fairly straightforward, and black market fentanyl has become a huge problem.
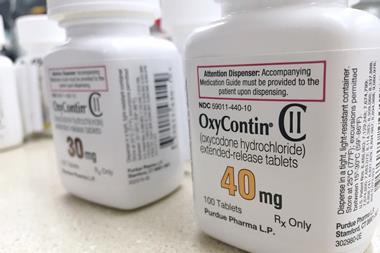
Perhaps the biggest cause of the spiralling problem was the sales tactics of opioid-producing companies. Connecticut-based Purdue Pharma was at the forefront. Its marketeers seized on a 1986 study in just 38 patients that claimed there were no health or addiction risks from long-term opioid use.1 Purdue sales reps started to aggressively promote its OxyContin slow release oxycodone formulation to physicians as a panacea for chronic pain. Backache? Osteoarthritis? Take OxyContin.
There’s a desperate search on for pockets of money to redress all the public harm caused, and this family sitting on, supposedly, billions of dollars is morally troubling to a lot of people
Another exacerbating factor was a campaign by the Joint Commission on the Accreditation of Healthcare Organizations (JC), a body that licenses many US hospitals and healthcare facilities. In response to a campaign from the American Pain Society that pain is the fifth vital sign (alongside temperature, pulse, breathing rate and blood pressure), in 2000 it directed that patients should be asked to rate their pain levels to ensure it was neither underassessed nor undertreated.
Doctors and nurses were pressurised to ask about pain. Patients were given an unrealistic expectation that they should have zero pain, and proffered high numbers on a scale of 0–10, even when their pain wasn’t actually that bad. The result? Yet more opioid prescriptions. While the JC backtracked on the pain survey in 2016, it has since been sued for exacerbating the crisis.
Legal landscape

The opioid litigation is currently on two different tracks, according to Harry Nelson, founding partner at Los Angeles-based law firm Nelson Hardiman. At the latest count, he says, the vast majority of the 1600 or so ongoing district court cases have been consolidated into a multi-district litigation in Cleveland, Ohio, with the first trials scheduled for October. ‘Both sides want to go to trial because of the expense and the risk,’ he says. ‘But it’s such an enormous undertaking, with so many issues, parties and pieces of evidence, that there will be strong pressure to reach settlement. I think there’s a good chance of a global settlement.’
The other track, he says, is state-based, and many state attorneys general have exercised their discretion to file lawsuits locally. The latest to be settled is in Oklahoma, for $275 million, Nelson says. This is unlikely to be the last.
The Sackler family, Purdue’s major shareholders, are also starting to feel the legal heat. In January, a complaint accusing family members of being behind the illegal marketing of OxyContin, written by Massachusetts attorney general Maura Healey, was unsealed by a state court judge. These documents revealed that at the launch party for OxyContin, Purdue’s Richard Sackler said a ‘blizzard of prescriptions’ would bury the competition. ‘[It] will be so deep, dense and white,’ he said.
New York’s attorney general has also filed a suit alleging that, over the past decade or more, the Sacklers have knowingly conveyed assets out of the US to protect them, and is going after these funds. Nelson believes other states will follow suit. ‘There’s a desperate search on for pockets of money to redress all the public harm caused, and this family sitting on, supposedly, billions of dollars is morally troubling to a lot of people,’ he says. ‘They’re certainly not the only ones, but it’s a compelling position that they shouldn’t be allowed to name medical centres and art galleries while so many millions of people have died and are struggling under the harm that they caused.’
The Sacklers’ lawyer, Mary Jo White, told Reuters in late April that the company is looking for a global settlement. She claims the litigation against them is ‘legally dubious, factually misleading and politically motivated’, and the crisis is a result of heroin from Mexico and fentanyl from China. ‘Let’s see what the real problem is and what the real solutions are rather than playing a litigation blame game with the fingers pointed in the wrong direction,’ she said.
In the big case in Cleveland, the plaintiffs’ lawyers and the attorney generals are now talking about multi-trillion-dollar settlements. ‘There has never been a trillion-dollar mass tort settlement; the biggest until now has been the tobacco litigation, which was nearer $200 billion,’ Nelson says. ‘Multi-trillion is a staggering number. It’s clear that Purdue alone and the Sackler family couldn’t sustain those kinds of numbers. This is why we’ve seen whispers Purdue itself initiated that it’s considering filing for bankruptcy.’
The settlements have already gone up dramatically. West Virginia was the first state to reach a settlement with Purdue, way back in 2004, for about $10 million. In 2015, Kentucky settled for $24 million. Oklahoma’s ups that by an order of magnitude. ‘How high can it go?’ Nelson says. ‘The attorney general of Oklahoma was looking for a much higher number, but the threat of bankruptcy, combined with the trial date, forced a number that both sides could live with.’ He believes the Oklahoma settlement reset the market, and a global settlement may happen later this year.
There has never been a trillion-dollar mass tort settlement; the biggest until now has been the tobacco litigation, which was nearer $200 billion
Purdue isn’t the only company to be sued. In a case in Massachusetts, for example, the founder and four employees of Insys were convicted of racketeering in early May. The company had inappropriately marketed Subsys, a sublingual spray formulation of fentanyl, to physicians. Other companies that have come under the legal spotlight for false marketing include Endo, Janssen, Allergan and Teva. ‘A whole series of companies that made opioid products [are being sued], but also the distributors, a handful of the large national pharmacies and insurance-related companies,’ Nelson says. ‘But OxyContin was the single most abused drug, so Purdue has been the most obvious target.’
A case against UK-headquartered Indivior points to a whole new trend, he adds – deceptive marketing around treatments for opioid addiction. ‘Indivior got into trouble for Suboxone, which is intended to be used as a treatment for opioid addiction, and it’s being heavily promoted as a form of therapy by the federal government,’ he says. He suspects Indivior will not be the last opioid treatment provider to come under legal pressure.
Nelson is, however, sceptical about how much all this litigation will actually help patients. ‘As always happens, the lawyers will do really well,’ he says. ‘A lot of money will go to states and cities who are looking to be reimbursed for their spending on overdose response.’ The academic sector is benefitting too – more than $100 million of the Oklahoma settlement went to fund a treatment and research institute at Oklahoma State University.
Agency action
Outgoing Food and Drug Administration (FDA) commissioner Scott Gottlieb described opioids as ‘the biggest public health crisis facing the FDA’ – and has accepted that the agency shares some of the blame. The FDA has committed to take more rapid action in the face of new threats such as the growth in illicit fentanyl, and to influence prescribing practices. ‘In this epidemic, waiting for the accumulation of definitive evidence of harm left us a step behind a crisis that was evolving quickly, and sometimes furtively, in vulnerable communities that were too often being tragically ignored,’ he said.
Several steps have already been taken, including updating the boxed warnings on products. Its risk evaluation and mitigation strategy (REMS) programme already required doctors involved in pain management to be trained in the safe use of opioids, and this has been expanded to other healthcare providers including nurses and pharmacists. It also now covers acute and chronic pain management, non-opioid and non-drug treatments, and addiction.

Of course, reducing the rate of new addictions will require fewer people to be exposed to opioids in the first place. The FDA says that as well as cutting prescription rates, the dose and duration of use should match both clinical circumstance and patient need. It is working with various stakeholders to develop evidence-based prescribing guidelines, and hopes to report back by the end of the year.
Tellingly, a 2017 study indicated that the likelihood of becoming opioid-dependent increases with the initial prescription’s duration.2 Patients given a five-day supply had a 10% risk of still using the drugs after a year. With a 10-day prescription, this rose to 20%. Those given a month’s supply at the outset had a 45% chance of still using the drugs after a year. Little wonder the federal government has proposed limiting the initial supply to just three days before a new prescription is required
Efforts to reduce prescription rates already appear to be having an effect: the FDA says that since 2015 the number of opioid analgesic prescriptions dispensed by outpatient retail pharmacies has dropped by 24%. Those for higher-strength products have fallen more steeply; by 2018, these accounted for less than 1% of all opioid units dispensed.
Online sales are another problem, and since 2017, the FDA has warned 23 networks operating more than 450 websites for selling products such as oxycodone and tramadol. Google now de-indexes websites based on these warning letters, while social media platforms such as Facebook and Instagram redirect those looking for online sources of opioids to the Substance Abuse and Mental Health Service Administration’s national helpline.
‘Cutting off this illicit internet traffic is critical,’ Gottlieb said. ‘We’ll continue to pursue all available means of enforcement to stop these online drug dealers.’ The agency has upped its inspection of imported packages to try and staunch the flow of products such as illegal Chinese fentanyl. Distributors are also to be held more responsible for securing the drug supply chain, to prevent diversion from legitimate supply.
The Substance Use-Disorder Prevention that Promotes Opioid Recovery and Treatment (Support) for Patients and Communities Act, passed last year, introduces another raft of measures. The FDA can now demand specific packaging to mitigate the risk of abuse or overdose, and is considering requiring immediate-release opioid tablets to be sold in the patient packs routinely used in Europe, rather than the tablets-in-bottle, counted out by a pharmacist, that are more typical in the US. ‘Small quantities in blister packaging, that comport with evidence demonstrating that a day or two of medication is sufficient, could reduce the overall amount of dispensed drugs available for misuse, abuse, and diversion,’ Gottlieb said.
The need for safer analgesics
Various abuse-deterrent products are already available, but current abuse-resistant dosage forms are rarely foolproof. Opana ER, Endo’s extended-release oxymorphone formulation, is a good example: the FDA made the company withdraw it in 2017 because it was being snorted and injected, despite its deterrence properties.
FDA is looking to address this, too. ‘We’ll advance new steps to promote the development of abuse-deterrent formulations of opioids by exploring new methods for analysing and evaluating abuse-deterrent features … and facilitating development of science for generic versions of these products,’ Gottlieb said.
Ultimately, more effective non-addictive pain treatments are required. The FDA plans to issue updated guidance for clinical endpoints and clinical trial approaches for non-opioid drugs in both acute and chronic pain. ‘Physicians don’t have good alternatives for patients with chronic pain,’ says Neil Singla, chief executive of US-based Lotus Clinical Research, which specialises in running trials on pain medications. ‘This is why it is important to develop new drugs – so physicians have real alternatives in their toolbox to help patients.’
However, developing effective pain drugs is not trivial. ‘Pain is a subjective phenomenon, so testing pain in clinical trials is really difficult,’ Singla says. It is inherently hard to measure – and it is challenging to run trials without a measurable endpoint that tells you whether it is working or not. ‘In clinical trials on drugs that are reformulations of [analgesic] drugs known to work, 50% still fail. That should not be the case!’ he says
Finding new, effective targets is a challenge, too, and many are being investigated. Two calcitonin-related gene peptide (CGRP) inhibitors – Aimovig (Amgen’s erenumab) and Ajovy (Teva’s fremanezumab) – were approved for migraine in the past year or so. Other targets under investigation include nerve growth factor (NGF) inhibitors and the Nav1.7 and Nav1.8 sodium channel blockers. These are still in the investigational stages and, while there has been some success, much work remains to be done.
Singla remains optimistic, however. ‘I think in the next five years there will be new drugs out there that are efficacious, and that will help solve the problem,’ he says. But it’s just part of the solution, along with education of both the public and physicians, and legal enforcement. ‘All of those things will help with the opioid crisis. But how do we prevent new people from becoming addicted?’
As Gottlieb says, ‘This is perhaps the biggest public health tragedy ever created through the deliberate actions of people. The opioid crisis took hold over the course of decades of action and inaction. Now, its scope is so large, and so devastating, its toll is self-evident. It will, unfortunately, take years of aggressive action to reverse its course for good. We won’t lose our focus on this fight.’
References
1 R K Portenoy and K M Foley, Pain, 1986, 25, 171 (DOI: 10.1016/0304-3959(86)90091-6)
2 A Shah, C J Hayes and B C Martin, MMWR Morb Mortal Wkly Rep, 2017, 66, 265 (DOI: 10.15585/mmwr.mm6610a1)















No comments yet