A dark red resin oozes from the trunk of Croton lechleri, giving the tree its Peruvian name, Sangre de grado: ‘dragon’s blood’. The people of the western Amazonian rainforest prize this tree for its medicinal properties, and they use it to treat everything from haemorrhoids to haemorrhaging. Bernabé Cobo, a Spanish missionary and naturalist who was posted to missions across Bolivia and Peru during the 17th century, was among the first to document its use. ‘This brew helps stop all kinds of incontinence and washing the haemorrhoids with it stops the bleeding common on them ,’ he wrote in his History of the New World. ‘The brew of its leaves and bark, when drunk daily, stops the flow of blood in the chest and stomach, and blood in urine.’ Sangre de grado can also be found in traditional remedies for gastrointestinal and circulation problems, staph, cancer and rheumatism. Cobo even described how, in a salty brew with Peruvian peppertree and wine, it’s used to treat gout. As for the sap, one of its most common uses is in dressings. The resin is daubed on open wounds, where it dries to form a blood-coloured latex seal that prevents infection.

Think some of this sounds like an old wives’ tale? Dragon’s blood is now a bone fide medicine. Six years ago, crofelemer, an extract from Sangre de grado sap, was approved by the Food and Drug Administration (FDA) in the US as a prescription drug for treating chronic diarrhoea in people with HIV. It’s the only antidiarrheal available that doesn’t interfere with antiretroviral medication and, apparently, it works – in clinical trials, 89% of patients on the two-pill-a-day regimen had a reduction in symptoms and over half had no diarrhoea at all after 20 weeks. Napo Pharmaceuticals, who market crofelemer as Mytesi, just signed a deal in the US with the Aids Drug Assistance Programs, which means people on low incomes in every state will be able to get it on the cheap.
Because it’s not a single molecule, crofelemer went via a slightly different route to get FDA approval compared to most drugs. The ‘botanicals’ pipeline allows drug makers to market mixtures of compounds from natural sources and takes into account any history of use in traditional medicine. Crofelemer is one of only two drugs to get approval via the botanicals route since the FDA first released its guidance for the process in 2004. So how does folklore become an FDA-approved treatment and why aren’t more traditional plant-based remedies making it?
The plants behind the pills
The fact that plants have a long history in modern medicine has not escaped today’s pharmaceutical chemists. Let’s return to Peru briefly for an example: quinine. Long before the advent of modern medicine, the Peruvians were fending off malaria with bark from the ‘quina-quina’ tree (now known as cinchona). According to legend, it was given as a cure to a Spanish countess who fell ill with the disease in Lima in around 1630.1 And it was Cobo again who was first to bring the bark to Europe. Quinine was eventually purified from the bark by French pharmacists and is still the next best option in areas of the world where other antimalarial drugs aren’t available.
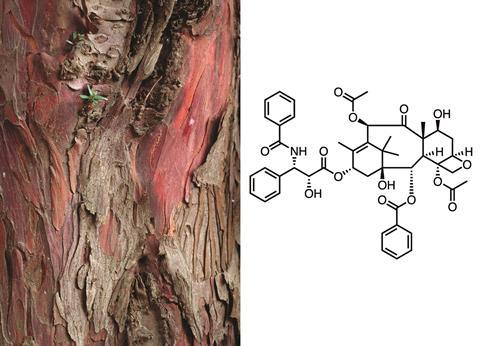
There are contemporary examples too, as Satyajit Sarker, director of the school of pharmacy at Liverpool John Moores University, points out. Several prominent cancer drugs come from plants, including paclitaxel (Taxol) from yew trees, and vincristine and vinblastine from periwinkle flowering plants. ‘They are a great success,’ he says. Despite this, only around 15% of plant species have ever been investigated and, according to Sarker, some that have already been dismissed could still yield interesting compounds with the help of modern separation and identification techniques. Microbes tend to be more popular sources, though most chemists who work on microbes could probably work on plants. ‘Once you have the extract, whether it is from microbes or plants, you have to test that extract in the same ways,’ he says.

With a quarter of a million plants to get through, working with those from traditional medicine at least provides a starting point, but even that’s a broad spectrum. For Sarker, the most reliable selection approach is a thorough search of the literature, which might include phytochemical databases and books on Chinese traditional medicines, as well as what we think of as ordinary scientific journals. Others favour field work. This was the ethnobotanical approach that led Steven King – today executive vice-president at Napo Pharmaceuticals – to pursue the promise of dragon’s blood for three decades. He is reported to have applied the sap to his savaged feet whilst working with Amazonian tribes in the 1970s.
Someone else who’s more comfortable in the field is Cassandra Quave, an ethnobotanist based at Emory University in Atlanta, US. She describes her approach as ‘using human knowledge of the environment’ to guide the search for medicine, though admits it may all seem a little ‘out there’ for some people’s tastes. ‘This whole thing where I go out and hike, talk to people in different languages and collect plants – I mean, that’s kind of weird for a lot of people,’ she says. But it’s led her to make some interesting selections.
Her current project is one that she’s now considering taking down the botanicals route. It began with a trip to southern Italy more than a decade ago, when she heard from locals about how they use sweet chestnut leaves in a rinse to treat inflamed skin. Sweet chestnut trees, the source of the chestnuts we roast and eat out of paper cones at Christmas markets, are found all over Europe. Their leaves are a little toothier and less broad than those of a horse chestnut. The Italian skin rinse piqued Quave’s interest because she knew that, in eczema, the sore patches of skin are a breeding ground for the bacterium Staphylococcus aureus. If extracts from this very common tree could take out staph, they might even offer a new strategy for tackling MRSA – the drug-resistant form. So she collected some leaves, dried them, and sent them home to the US in a vacuum-sealed bag for later analysis.
Fruity fractions
However you get your hands on the plants, it’s at this point that the serious business of phytochemistry begins. ‘It’s a long process,’ Sarker explains, and a repetitive one involving extraction, fractionation and testing of the various fractions for activities that could be important in disease. In traditional remedies, crude extracts or infusions might work wonders, but for chemists, it’s all about refining down the extract to the smallest possible number of compounds that have an effect and trying to work out exactly how those compounds interact with cells. The bioactive ones will often be plant secondary metabolites; molecules with some non-essential role in the plant.
The first principle of any anticancer drug is that it will have to kill cells
Generally, the process starts with grinding the plant material into a fine powder to increase the surface area, then extraction using solvents of increasing polarity. The initial extractions get rid of the oily and fat-linked compounds, leaving polar compounds like the flavonoids, tannins and lignins to the methanol extract, usually the most active portion. However, each has to be tested. As one of Sarker’s main focuses is anticancer compounds, his starting point is often a cytoxicity – cell-killing – assay. ‘The first principle of any anticancer drug is that it will have to kill cells,’ he says. ‘So we do the assay to find out which one of these extracts is active.’
By now, the number of different molecules has shrunk significantly but it’s still too many to deal with. ‘You have one total methanol extract, which contains maybe 100 to 200 compounds,’ says Sarker. ‘So now we have to fractionate them according to the various chemical groups.’ They do this using solid phase extraction, working from low concentrations to high concentrations of methanol in water, to produce different fractions that are again dried and tested to find out which is active. Then it’s down to high-performance liquid chromatography (HPLC) to separate the compounds from the active portion. Finally, when they’ve narrowed down their candidate compounds to around 10–15, they start using spectroscopic techniques like nuclear magnetic resonance (NMR) and mass spectroscopy to identify them, confirming which ones are responsible for the plant’s medicinal properties with yet more activity tests.
Sarker’s team recently went through a version of this process with some small reddish-orange fruits picked up in a market in Dschang, Cameroon.2 The dried fruits of ‘sand knobwood’ (Zanthoxylum leprieurii) are made into infusions for treating sickle cell anaemia but are also notable in the scientific literature for containing compounds with anticancer and antimicrobial activities. The fruit extracts yielded five diterpene compounds, one of which wiped out 92% of human prostate cancer cells in a cytotoxicity assay. Spectroscopic data confirmed it was kaurenoic acid, a molecule with known painkilling, anti-inflammatory and antioxidant activities, but it was the first time the compound had been isolated from the tree or any of its relatives in the genus Zanthoxylum. What’s satisfying about this work is that it can validate the medicinal benefits of plants that are already widely used in traditional treatments. From here, Sarker hands over any potential lead compounds to other groups or companies that carry out animal testing, where the task of developing an anticancer drug based on a single molecule can begin in a fairly typical way.
In the mix
However, it’s not always possible to nail a single molecule that’s responsible for a plant’s beneficial effects. At the time of writing, Quave is still working on isolating active compounds from sweet chestnut. After the vacuum-sealed leaves arrived from Italy, the Emory team worked hard on making its extracts and separating them into various fractions, but soon discovered that they were useless at killing staph. For Quave, this was just an incentive to start thinking further outside the box. Eventually, in a 2015 paper in PLoS ONE,3 she and her team showed the surprising way in which a plant that has no power to kill MRSA could stop it causing harm. Instead of destroying the bugs, like conventional antibiotics, sweet chestnut stops them communicating. Although they couldn’t pinpoint the exact mechanism, or compound, Quave’s team showed that something in the most potent portion of their extract (labelled 224C-F2) was inhibiting staph signalling molecules involved in triggering bacterial toxin production. This same portion also reduced the size of skin ulcers in mice infected with MRSA. Ironically, the fact that 224C-F2 doesn’t actually kill staph is what makes it such an exciting prospect, because it may exert less pressure on the bug to adapt and develop resistance.

The implication is that Quave may have found a whole new way to treat staph infections, but because she’s still working with a mixture of plant molecules she’s going to have some tricky decisions to make; whether to go down the botanical route to getting a treatment approved, or the ordinary one. ‘I’m torn in two directions here,’ she says. ‘On the one hand, we can create an enriched extract that works really well in vitro and also in animals, and there is a drug development pathway for that. On the other hand, to make this really amenable for, perhaps, joint therapy with antibiotics in the future, the best scenario would be to isolate a single compound.’
With botanicals, it’s most likely that it’s a group contribution
If she did go down the botanicals route, 224C-F2 would be thrown into a pipeline with at least 600 other botanicals registered as investigational new drugs since its inception – with only crofelemer and a genital warts product, sinecatechins, having seen the light of day so far. According to the FDA, only 2% (so roughly 12) of these potential products have made it to phase III clinical trials thus far. The proportion of ordinary investigational new drugs that make it is 23%, although it’s difficult to make comparisons given that so few botanical drugs have gone through the whole process.
There is an argument for going down the botanical route in cases where an extract is safe and does a decent job, especially if it appears the composition or mixture works better than any single compound that it contains. ‘With botanicals, it’s most likely that it’s a group contribution; that individual isolates may not work,’ explains Laird Forrest, a pharmaceutical chemist at the University of Kansas in the US. ‘It’s more a synergy between all of them together.’ Which brings us back to dragon’s blood.
While some of the early studies on crofelemer put its antidiarrheal activity down to a molecule called SP-303, a precursor to the drug,4 Forrest’s recent work for the FDA shows there are many different chemical structures that have a similar effect.5 The crofelemer molecule itself is a type of polyphenol called a proanthocyanidin that is made up of catechin (a type of flavonoid) subunits linked together in a polymer chain. In the extract made from the Amazonian tree sap, however, the number of catechin units in each chain varies wildly, depending on aspects such as the particular grove of tree that the sap was sourced from, how it was harvested and even what season it was harvested in. There could be anywhere between one and 28 catechin units per chain and, according to Forrest, they all work. ‘We found, actually, anything works – even the monomers,’ he says. ‘We analysed several available batches of crofelemer and they were very, very different on the basis of chemistry and size, but they all appeared to work the same by our in vitro assays.’
No one knows why these random mixtures of crofelemer chains work, because no one really knows exactly how crofelemer works. The same is true of the other approved botanical, sinecatechins, which is also catechin-based. Crofelemer apparently reduces diarrhoea by targeting chloride channels in gut cells that are involved in triggering the passage of water through the bowel,6 but the exact nature of its interactions with chloride channels remains unclear.
Weighing it up
It’s because of the problems with variability that Sarker remains unenthused about pursuing extracts as medicine. Crofelemer is considered a relatively safe drug because it passes through the intestines without being absorbed, but Sarker says some potential botanical products could do great harm. ‘There are so many variables,’ he says. ‘Unless they are controlled properly, it is really dangerous, because some plants growing in different places may have different compositions of compounds. The balance between toxicity and efficacy may shift and that may produce unnecessary side effects, or even kill patients.’ Unfortunately, it may be the only cost-effective option for drug development in countries with limited resources for R&D.

For a scientist in a rich country, it’s more about weighing up the best way to get your treatment to market when it’s more complex than a single molecule. Mixtures, in particular, are a headache. As Quave explains, doing all the pharmacology on one compound is hard enough; add in one more, plus the pharmacology on both together, and things are already very complicated, never mind if you want to mix up, say, five. And that’s if you know what all the important compounds are.
For those who do end up going down the botanicals route, it’s not much different to the regular one. According to the FDA, botanicals are given some ‘flexibilities’ in the early phase trials given previous use in humans but the process is otherwise the same as it is for all drugs. As Jeremy Kahn, a spokesperson for the Center for Drug Evaluation & Research at the FDA, points out, botanicals do have some additional issues that can frustrate the process. ‘Botanical mixtures often contain small and large molecules, and there are often challenging issues surrounding analytical method and reference standard development.’ He lists raw material and manufacturing process control, and batch-to-batch consistency, as additional challenges. How can you tell, for example, if the correct plants have been harvested, or if they’re suddenly being imported from a completely different country?
The FDA is trying to address these problems. When it commissioned Forrest’s crofelemer studies, it was trying to learn something more general about how to test batch quality in botanicals. The trouble with modern analytical techniques is that there are a lot to choose from, so the FDA wanted ways to establish the fewest possible number of tests that could determine quality. Forrest’s approach was interesting because he uses machine learning. Put simply, he uses computers to look at large amounts of data and pick out what’s critical; in this case, the tests that are going to determine quality. ‘[The FDA] told us that they do plan to incorporate this type of machine learning into development programmes in the future,’ says Forrest.
Time is a healer
If crofelemer is anything to go by, getting a botanical through the FDA is not exactly a breeze. The normal approval process is said to take an average of 12 years. After being granted ‘fast-track’ designation in 1998, crofelemer suffered issues of ‘identity and potency’ (in Forrest’s words) before eventually being approved 14 years later, by which time its original backers, Shaman Pharmaceuticals, had filed for bankruptcy.
The plants that had some effect became traditions that were passed down and refined over the centuries
For now, Quave is continuing the hunt for a single active molecule in sweet chestnut, though she’s bearing in mind ‘what’s really feasible for getting these drugs out to people through frameworks that currently exist for approval and manufacturing’. Getting to the root of how some of these traditional medicines work can be a trial, even with all the tools of modern medicine. Yet, for hundreds of years, communities developed practical treatments based on the only thing they had at their disposal: nature. As Quave points out, they were immersed in it ‘on a daily basis’; they tasted the plants, smelled them and saw how animals interacted with them. Aside from that, there’s no underestimating the importance of time. ‘For those [plants] that had some effect, over the centuries, they became traditions that were passed down and refined,’ says Quave. ‘Knowledge was spread, just like in the western medical systems that we have today.’
Hayley Bennett is a science writer based in Bristol, UK. Spanish translation by Adriana Castro
NOTE: Article updated on 17 September 2018 to correct structure of kaurenoic acid and remove incorrect structure of Crofelemer
References
1 A R Butler, S Khan and E Ferguson, J. R. Coll. Physicians Edinb., 2010, 40, 172 (DOI: 10.4997/jrcpe.2010.216)
2 S T Guetchueng et al, Rec. Nat. Prod., 2017, 11, 304 https://bit.ly/2JLK4wn
3 C Quave et al, PLoS ONE, 2015, 10, e0136486 (DOI: 10.1371/journal.pone.0136486)
4 M Holodniy et al, Am. J. Gastroenterol., 1999, 94, 3267 (DOI: 10.1111/j.1572-0241.1999.01535.x)
5 P A Kleindl et al, J. Pharm. Sci., 2017, 106, 3242 (DOI: 10.1016/j.xphs.2017.07.012)
6 L Tradtrantip, W Namkung and A S Verkman, Mol. Pharmacol., 2010, 77, 69 (DOI: 10.1124/mol.109.061051)














No comments yet