An HIV vaccine may not be available anytime soon, but its proponents are hard at work, reports Dinsa Sachan
Long-time HIV activist Bill Snow is now retired but the lack of an HIV vaccine still plays on his mind. Snow was one of the first people to campaign for such a vaccine when HIV was discovered, even though there was more focus on developing a treatment at the time. ‘I experienced the transformative power of the polio vaccine in the 1950s,’ says Snow. ‘A vaccine was also behind the eradication of small pox, the first disease to be eradicated.’
The hunt for an HIV vaccine has now entered its fourth decade. ‘I thought we’d be closer to a vaccine by now,’ he concedes. Snow is almost 70 now. Despite the slow pace of research, he is still confident there will be an HIV vaccine in his lifetime.
A preventative measure

Even though there’s effective treatment (antiretroviral drugs, ARV) as well as prevention options – condoms, circumcision and oral pre-exposure prophylaxis (ARV drugs taken to prevent infection in high risk populations) – available to fight the disease, the world is nowhere near eradicating it.
In 2016, 36.7 million people worldwide were living with HIV. Thanks to ARV therapy, 13.1 million HIV-related deaths were averted from 2000 to 2016. A recent UN report found that new infections have increased in several parts of the world. In Eastern Europe and central Asia, there was a 57% increase in annual new infections reported from 2010 to 2015. Similarly, rates have soared in many parts of Africa, the continent that has the biggest Aids epidemic.
We have never ended an epidemic without a vaccine
Mitchell Warren, AVAC
Advocates think an HIV vaccine is the need of the hour. ‘We have never ended an epidemic without a vaccine,’ says Mitchell Warren, executive director of the US-based not-for-profit AVAC, previously known as Aids Vaccine Advocacy Coalition. ‘Even if we get everyone on antiretroviral treatment, deliver pre-exposure prophylaxis drugs and circumcise, it’s not enough to sustain the end of the epidemic.’
Stumbling blocks
Scientists have been looking for an HIV vaccine for nearly as long as we have known that HIV causes Aids. The first attempted approach in beating the virus was to encourage the body to make antibodies that targeted the outer glycoprotein envelope of the virus. These glycoproteins bind to healthy immune cells and establish the infection. Blocking this process should theoretically prevent the virus taking hold in the body.
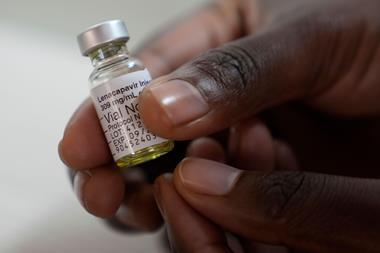
The first Phase III study using this approach began in 1998. On trial was the vaccine AidsVax. Created by the San Francisco, US-based pharmaceutical company VaxGen, it consisted of genetically engineered proteins similar to gp120, a glycoprotein found on the rim of the HIV virus. The vaccine was tested on more than 5000 participants across North America and the Netherlands who were mostly men who have sex with men (including both homosexual and bisexual men) and women whose lifestyle made them susceptible to infection. In 1999, a second study kicked off in Thailand, to test a similar vaccine in 2500 South East Asian participants, all of whom were drug users. Both these vaccine candidates failed to prevent HIV infection in their subjects.
Another approach was tried using a different arm of the immune system: cell-mediated immunity. The protagonists of this mechanism are T-cells, a type of white blood cell. Unlike antibodies, they don’t fight off the pathogens as soon as they enter the body. T-cells work by destroying cells that have already been hijacked by a pathogen.
None of these infected T-cell targeting candidates reached the Phase III stage. Two Phase IIb trials of the US pharmaceutical giant Merck’s recombinant vector vaccine, for example, were stopped in 2007. In one of the trials, the vaccine had actually increased the risk of infection. The scientists had introduced genes of the HIV virus into a live common cold virus, which had been disabled so it didn’t cause illness. Once inside the body, these HIV genes should express themselves as antigens similar to those produced by the actual HIV virus. These antigens should then activate the T-cells and prepare the body to fight the HIV virus in the future.
Finally, a breakthrough
The ongoing phase of this field is ruled by combination strategies. The three-year trial RV144, led by the US military and the Thai government, defined this new wave in the hunt for the HIV vaccine. Starting in 2003, the Phase III trial was held in Thailand and enrolled more than 16,000 participants.
The vaccine had two parts: prime and boost. The prime – Alvac – is a type of recombinant vector vaccine. The vector is a weakened form of canarypox virus that causes disease in birds. It carries three genes of the HIV virus and introduced them into the immune system of the person receiving the vaccine. The boost was the AidsVax vaccine, the same one used by VaxGen. The participants received six sets of shots – four of Alvac and two of AidsVax – over a six-month period.
The RV144 trial gave us a lot of hope
Linda Gail-Bekker, Desmond Tutu HIV Centre
In 2009, the RV144 researchers announced that the vaccine regimen was safe and 31.2% effective in preventing HIV infection compared to placebo. These figures weren’t mind-blowing, but it was the first time a vaccine candidate had worked. ‘The RV144 trial gave us a lot of hope that it is feasible to create an immune response that will stop virus acquisition at least for the short term,’ says Linda Gail-Bekker, a researcher at the Desmond Tutu HIV Centre at the University of Cape Town, South Africa.
After the RV144 trial, several organisations and institutions, including the US military, joined forces to form the Pox-Protein (P5) partnership. This coalition has been carrying out follow-up studies to learn more about why the RV144 vaccine worked – and why it only worked in some people.
Follow-up studies have been enlightening for the research community. Recently, the US military announced results of their follow-up trial: RV305. It involved 162 HIV negative participants from RV144. Six to eight years after the original trial, they were given a boost of either AidsVax, Alvac or both combined.

The researchers found that participants who had received an AidsVax boost produced a higher amount of antiHIV antibodies. Even after all that time, there was ‘strong immunologic memory’, says Sandhya Vasan, who is a researcher with US Military HIV Research Program (MHRP) in Bangkok, Thailand, and the lead researcher of the study. ‘This study showed us that responses in RV144 are able to be boosted,’ she says. ‘The disappointing aspect was that they still go away.’ The challenge now is to figure out how to make the antibodies stick around for longer.
In another study, RV306, MHRP and collaborators gave 360 participants in Thailand the RV144 vaccine regimen over a six-month period and then different groups received boosts at months 12, 15 and 18. Improved immune responses were seen in those receiving the booster shots. Vasan speculates that, based on these findings, the answer to the HIV puzzle may lie in a serial vaccine strategy– ‘sort of like an annual flu shot’.
Meanwhile, a Phase IIb trial of the recombinant DNA-based vaccine HVTN505 was stopped in 2013, because the group that received the series of vaccine acquired more infections compared to the placebo arm. Nonetheless, RV144’s success gave the field a new vigour.
It’s absolutely the most exciting time in HIV vaccine research
Mitchell Warren, AVAC
The way forward
Currently, this research area is buzzing with activity. ‘Right now, there is more happening in clinical trial and in basic science than ever before,’ Warren says. ‘So it’s absolutely the most exciting time in HIV vaccine research.’
Vaccine enthusiasts are eagerly watching as a big efficacy trial, called Uhambo (meaning journey in Zulu) is being conducted in South Africa. Starting in 2016, it has recruited more than 5000 volunteers. The vaccine candidate is similar to RV144, but has key differences chemically. Gail-Bekker, who is a principal investigator in the study, says these differences make it more ‘robust’. It’s specifically targeted at Clade C, the HIV strain that is prevalent in South Africa, with participants receiving five injections over a period of a year.
And it’s not just researchers who are excited. ‘People are very willing to participate,’ says Gail-Bekker. ‘This is a heavily burdened country, a lot of people are affected by HIV, and so they really want to help find solutions.’ The results of Uhambo are expected in 2020.
Meanwhile, Janssen, the pharmaceutical arm of Johnson & Johnson, is placing its bets on prime-boost vaccine candidate HIV-V-A004. First, a disabled common cold vector is being used to express a group of synthetic HIV sequences designed to boost the immune system. These optimised versions of sequences that code for natural proteins are called mosaic sequences. Then, a purified HIV envelope protein is given to boost the effect of the prime vaccine.
These synthetic HIV sequences are designed to be able to garner an immune response from a broad range of HIV strains. Four Phase I or Phase II trials are currently being conducted across the globe testing various regiments related to the vaccine. ‘The objective is to move the best vaccine candidate into larger scale Phase IIb study this fall,’ says Dan Barouch, director of the center for virology and vaccine research at Beth Israel Deaconess Medical Center, Boston, US.
A Pandora’s box
Broadly neutralising antibodies offer another potential approach to fighting a broad range of HIV strains. These antibodies are designed to lock themselves to certain parts of the HIV virus and stop its replication.
Seven years ago, the antiHIV antibody VRC01 was discovered in the blood of an HIV patient who had been able to keep their infection in check without treatment for over a decade.
The antibody has been has been synthesised in the lab and proved able to ward off HIV infection from 90% of strains prevalent around the globe – in a petri dish. Since 2016, the potential of VCR01 to prevent HIV infection has been being tested in a large Phase IIb clinical trial spanning three continents.
We are taking the first step of a very long road … so far, the walk is pretty good
Myron Cohen, HIV Prevention Trials Network
The trial participants are receiving intravenous infusions of VRC01. But ultimately, Cohen hopes that it will be possible to develop a vaccine that could induce this antibody in the body. ‘We are taking the first step of a very long road,’ says Myron Cohen, a principal investigator at HIV Prevention Trials Network, one of the organisations running the trial. ‘So far, the walk is pretty good.’
A stubborn enemy
While the current developments in the field are exciting, the long fight to beat HIV has definitely worn the community down a bit. ‘We’re frustrated at some level that we don’t have a vaccine yet,’ says Vasan. ‘But I don’t think it’s for lack of trying or momentum from the scientific community.’ It turns out that HIV is just a very tough virus to beat. ‘This vaccine is asking us to do what no vaccine has ever asked us to do,’ says Barton Haynes, a professor of medicine and immunology at Duke University, US. ‘HIV is rapidly mutating and its vulnerable spots are well protected and tough to infiltrate.’
A vaccine essentially helps teach our immune system to prevent infection, explains Warren. ‘HIV is a virus that is destroying the very cells that you’re trying to teach to fight off infection, that is different than any other diseases,’ he says. ‘Because we’re trying to give a vaccine to the actual cells that are being destroyed by the virus and that’s why an HIV vaccine is so much more complicated than some of the other diseases.’
Even though overall funding for HIV prevention efforts has declined, cash for HIV vaccine research has remained stable over the years. In 2015, this field garnered funds up to US$862 million – a 2% rise from 2014. However, things might change with the proposed budget cuts to the US National Institutes of Health, the biggest funder of HIV vaccine research. ’We are very concerned about any stepping back that may affect the development of a safe and effective HIV vaccine,’ says Mark Feinberg, president of the not-for-profit International Aids Vaccine Initiative. ‘It will definitely slow down the time in which an HIV vaccine will be available and that will translate to many more people getting infected with HIV and many more people dying.’
As the scientific community speculates the budget cuts, there are other challenges that it faces. ‘Most vaccines are developed in the private sector by pharmaceutical companies which have lots of experience developing vaccines and know about the reality of product development,’ says Feinberg. But much of the discovery work for HIV vaccines is coming from academia – and that’s a problem. ‘They may have great ideas but they don’t have experience to develop vaccines and get them licensed,’ says Feinberg. ‘So there is a real need to figure out how different stakeholders can work together to be more efficient.’
A functional cure
Right now, scientists are consumed with the search for a so-called preventive HIV vaccine that will prevent the virus from spreading infection in the body. But work is also ongoing to find a therapeutic vaccine that helps the body fight HIV infection in a person that’s already infected. A therapeutic vaccine, also known as a functional cure, would help reduce patients’ viral load and their reliance on ARV drugs.
The field of therapeutic vaccines has grown slowly compared to preventive vaccine research. But a few Phase I and pre-clinical studies have provided hope. In 2016, a study published in Nature described a therapeutic vaccine that, when given in combination with another drug, reduced viral load of Simian immunodeficiency infection in rhesus monkeys. In three out of nine animals, the virus was undetectable. ‘These data demonstrate the potential of therapeutic vaccination combined with immune stimulation as a strategy aimed at a functional cure for HIV-1 infection,’ wrote lead author Dan Barouch of Beth Israel Deaconess Medical Center, Boston, US.











No comments yet