MOF delivers cancer drug candidate straight to mitochondria
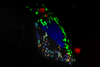
New ‘Trojan horse’ strategy could reduce drug doses needed to kill cancer cells
A metal-organic framework (MOF) has been created to effectively smuggle drugs into mitochondria, which are where cancers often begin. The researchers have also revealed the mechanism cells use to ‘swallow’ MOFs – an important first step towards developing more efficient drug delivery systems.1
