James Mitchell Crow explores the next generation of therapeutic biomaterials, which aim to interact dynamically with the body and help to control diabetes and heal wounds
Benjamin Almquist wants to take biomaterials into the fourth dimension. Almquist’s lab, in the bioengineering department at Imperial College London in the UK, is developing materials that dynamically interact with the body to promote wound healing. It’s just one area of medical need where biomaterials that can react to biochemical cues in their changing environment could make a big difference to patients’ outcomes.
Wound repair is a case in point. This complex multi-step process involves waves of different cell types to kill off infection, clean away damaged cells and then form new tissue. There are plenty of places the process can get derailed, with outcomes ranging from chronic wounds that fail to heal, to excess scar tissue formation.
Today’s clinically approved wound-promoting materials are passive participants at best, such as controlled release materials that release their therapeutic cargo at a pre-programmed rate. ‘Those materials don’t actually interact with what is happening during wound healing,’ Almquist says. ‘It’s like dancing and somebody changes the pace of the music but you keep dancing at your original speed.’
Glucose control is trickier than it sounds
Almquist is one of a growing number of researchers looking to develop materials that are a bit more agile on their toes, responsive to the changing rhythms of complex biological processes happening around them.
Sugar highs
Some of the longest-sought smart biomaterials are designed to autonomously maintain healthy blood glucose levels in people with diabetes, by continually sensing glucose concentration and releasing tailored insulin doses in response. If a smart, long-lived yet fast-acting glucose-regulating material could be developed, the more than 400 million people with diabetes worldwide could directly benefit. The technology could also become a model system for smart materials that dynamically release any drug in response to a specific biological cue.
Glucose-sensing insulin-releasing biomaterials may be simple in concept, but it is proving highly technically challenging to get the chemistry working right. ‘Glucose control is a very big area with a lot of work going on, but glucose control is trickier than the idea sounds,’ says Almquist. ‘It has to happen continuously, all day every day, and has to be sensitive and fast enough to respond.’
The first example, developed in 1979, was based on a glucose-binding plant protein called concanavalin A (ConA). The protein was incorporated into a polysaccharide matrix that was loaded with insulin. In the presence of free glucose, ConA-glucose binding would trigger dissociation of the ConA-polysaccharide matrix, releasing insulin.
This system wasn’t successfully brought into use, mainly because the ConA protein triggered immune system side reactions in recipients, but it set the general blueprint that most attempts have followed. The insulin is encapsulated in some form of matrix – usually a hydrogel – and released by a chemical glucose recognition event.
Hydrogels are three-dimensional networks of cross-linked hydrophilic polymers that soak up large amounts of water. They are an ideal biocompatible blank canvas for building reactive biomaterials. ‘They can encapsulate living cells, they can encapsulate a variety of bioactive and biological therapeutics – including proteins, because they present an environment that preserves protein structure,’ says Cole DeForest, who develops smart biomaterials at the University of Washington in Seattle, US. By changing the polymer or the cross-linkers that hold the polymer network together, they can be made to release their cargo in response to a vast range of biological cues.
In the case of insulin release, one strategy has been to use hydrogels that collapse or swell in response to changing pH, and to incorporate the glucose oxidase enzyme as their glucose-sensing component. Glucose oxidase turns the sugar into gluconic acid, dropping the pH to trigger insulin release from the hydrogel.
It should be possible [to control glucose levels] at human scale using the microneedle system
These systems have generally been too slow for effective glucose control, especially in the pH-buffered environment of the body. But another glucose-sensing moiety, phenylboronic acid (PBA), looks far more promising for practical hydrogel-based insulin release under physiological conditions. ‘The interaction between glucose and boronic acid has been known for almost 100 years,’ says Akira Matsumoto, a biomaterial engineer at Tokyo Medical and Dental University in Japan. PBA reversibly binds glucose in an equilibrium reaction – and therefore has the potential to act as a switch turning insulin release on and off.
Matsumoto is part of a team that, in the 1990s, demonstrated an insulin-releasing hydrogel based on phenylboronic acid. At high glucose concentrations, the PBA side chains along the hydrogel’s amphiphilic acrylamide polymer backbone bind glucose, forming a charged, fully hydrated state that releases insulin. As glucose concentrations fall, and less and less glucose remains bound to the PBA, the hydrogel reverts to an uncharged state and begins to dehydrate. When glucose concentration reaches the target level, a skin layer forms rapidly across the hydrogel surface that shuts off insulin release within seconds.
After years of work, fine-tuning parameters such as the ratio of PBA units in the acrylamide backbone, the team developed a system that works at physiological temperature and pH, and is tuned to maintain glucose concentration to within normal levels.1 The material is performing well in animal models. ‘Our system is excellent at controlling daily blood glucose fluctuations,’ Matsumoto says. ‘We have very acute response, a manner of 10 seconds, and can sustain this performance for a week. People don’t have that technology yet, so we are very excited.’
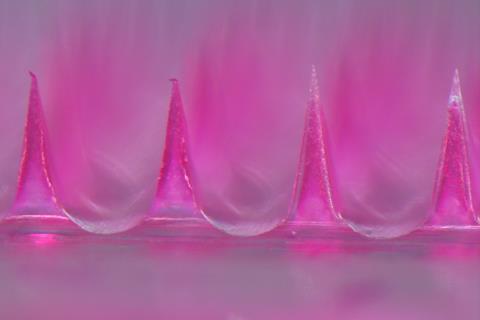
Using a catheter and an external reservoir of the hydrogel, the material kept glucose levels under control for three weeks in diabetic mice. The team has since seen similar success in rats, which are 10 times the bodyweight of mice. Most recently, Matsumoto published results showing that microneedle patches coated with the hydrogel could control glucose levels in mice for a week.2 ‘As it is a diffusion-based system, the challenge is to scale it up to increase the power of the device [for larger animals and humans]. We have to increase either the surface area or the concentration gradient,’ Matsumoto says. ‘Using the microneedle system, it should be possible for human scale,’ he adds. The team’s next goal is to use their microneedle patches to achieve sustained glucose control in pigs, which have a similar body mass to humans.
Heartening developments
Jason Burdick at the University of Pennsylvania in the US is one of the pioneers in the therapeutic smart hydrogel research space. First-generation drug-releasing hydrogels, incorporating polymers such as poly(alpha-hydroxy esters) that are sensitive to hydrolysis under physiological conditions, can only release an encapsulated therapeutic at a pre-engineered rate. Burdick developed hydrogels in which therapeutic release rate is dynamic, depending on the levels of a specific enzyme.
‘Enzymes often change in response to disease – for example, matrix metalloproteinases (MMPs) are largely increased in tissues after a heart attack,’ Burdick says. As elevated levels of these protein-degrading enzymes cause permanent damage to tissue structure, there has been ongoing research to try to develop MMP inhibitors. But none has been successful in people, due to off-target side effects.
Burdick developed a more targeted strategy.3 ‘Our approach is to design hydrogels where the crosslink in the hydrogel network consists of peptides that degrade in response to the MMP enzyme,’ he says. ‘It is an “on-demand” approach, where an increase in the enzyme levels with disease will release inhibitors to block the activity of that same class of enzymes.’
After successfully testing their injectable on-demand MMP-targeting hydrogel in a pig model of heart attack, Burdick and his colleagues started a spinout company, Prohibix, to translate the technology to biomedical applications. ‘We are pursuing cardiac applications, as well as other diseases,’ Burdick says. ‘We hope that it can translate to the clinic.’
A logical approach
Plenty of triggers besides MMP are being explored. ‘Light is very interesting, since there is great control over where and when you introduce the light,’ Burdick says. ‘There is great work on photo-responsive hydrogel materials from groups such as Kristi Anseth [at University of Colorado], Andres Garcias [at Georgia Tech] and others that allows light to trigger material changes.’ Crosslinkers that incorporate ortho -nitrobenzyl esters undergo photoscission of the ester bond when irradiated with near-UV 365 nm light. Alternatively, the crosslinker can incorporate disulfide bonds, which cleave under reducing conditions often associated with disease.
In Seattle, DeForest and his team are incorporating all of these triggers into the same hydrogel, to create biomaterials that exploit programmable Boolean logic to exert even tighter control over when and where the hydrogel’s cargo is released.4
We can independently and sequentially control their release
‘We realised that most of the cues people were using to induce these material responses, to release a therapeutic in a “local” way, were pretty far from unique,’ DeForest says. The less unique the trigger, the greater the chance the material would have off-target effects, and the lower its chance of passing clinical trials. ‘We thought, can we come up with a generalisable strategy that would require not just one of those cues to be present, but two?’ DeForest says. ‘Even if each of those cues individually is not super-specific to a given location, maybe the combination of them would be more specific than either of them alone.’
Logic gates enable this multi-cue sensitivity, DeForest has shown. A hydrogel crosslinker that cleaves in response to a single cue – such as an MMP enzyme – is effectively functioning as a YES gate. If an MMP-sensitive group is connected in series with a dithiol group, so that if either cleaves the crosslink is broken, that crosslink is behaving as an OR gate. If the MMP sensitive group and the dithiol group are connected in parallel, in a cyclic structure that requires both groups to be cleaved to break the crosslink, that’s an AND gate.
‘DeForest’s group has been turning up some really fascinating work,’ Almquist says. ‘Their materials with Boolean logic capabilities can take multiple stimuli that give you different outputs based on what the stimuli are.’
Although the logic gate idea was not completely unprecedented, DeForest has been systematically making and testing all the possible logic gate combinations. ‘The big jump we tried to make was to make it fully modular,’ he says. ‘We weren’t developing a single scheme, but a set of design criteria that, if you follow them, you can substitute in any degradable linkages, and get a material that is responsive to any different combination of inputs.’
To target cancer, for example, DeForest and his team developed materials that only release their therapeutic cargo in the presence of MMPs and a chemically reductive environment, both of which are characteristic for tumours. ‘We are taking advantage of requiring both of those cues to elicit delivery of a therapeutic to locally kill off tumour cells.’
Most recently, the team has developed their logic gate multi-cue concept to produce a single hydrogel that contains three different protein therapeutics, each released by a different pre-programmed set of cues.5 ‘These are full-length proteins, site-specifically modified with these linkers, so we can independently and sequentially control their release.’ The team is currently testing these materials for wound healing, with the idea of sequentially releasing proteins in response to cues naturally presented in different phases of wound recovery.
So far, the team has been using easily-characterised macroscopic gels, tested against cell cultures. ‘We’ve been working on formulating these logic degradable systems in a nanogel formulation that can be administered through IV administration.’ The team can then carry out mouse studies for in vivo validation of the strategy.
Healing wounds
Light can offer precise external control over a smart hydrogel matrix, but it has some obvious limitations. DeForest is looking toward red-shifted chemistries, developing linkers sensitive to the lower wavelengths of light that can penetrate further into the body. ‘There have also been innovations on the electrical engineering side of things, from the optogenetics community, using fibre optics to deliver certain wavelengths of light at certain times,’ he says. Even so, light might be useful for research, but is not going to be generally applicable for medical use. ‘Realistically, when we are thinking about trying to make a material that’s going to have therapeutic relevance in humans, we think of light as just a model input. We are trying to move away from that for materials to be used deep inside the body.’
At Imperial, Almquist is also looking for ways to move away from exogenous triggers such as light, and exploit more natural cues that the body is already using to orchestrate complex processes such as wound healing. ‘We look to natural systems to see how they function, and see if we can recapitulate some of that behaviour,’ Almquist says.
Almquist has developed a system that responds to a physical cue.6 During wound healing, a growth factor called TGF-b gets laid down along with the newly re-laid tissue scaffold called the extracellular matrix (ECM). ‘This scaffolding is soft, but over the course of wound healing becomes stiffer and stiffer,’ Almquist says. Cells called myofibroblasts pull on the ECM to stiffen it up. Once stiff enough, the myofibroblasts can grab onto the protein cage the TGF-ß is wrapped in, releasing and activating the growth factor. ‘This sets up a feed-forward loop that tells the cells doing this matrix remodelling to do more of it,’ Almquist says. The contracting ECM closes the wound.
Using traction forces to release growth factors is a unique cue found only in wound healing – and so a unique trigger that smart biomaterials could use to help promote it. The trick to exploiting traction forces in this way is to use short chemically synthesised single strands of DNA called aptamers, Almquist showed. These can be tuned, via directed evolution techniques, to fold up into a specific 3D shape to bind to a target substrate. ‘When they are folded they can fit into a binding pocket on a protein. But if you straighten them out they lose all of their binding affinity,’ Almquist says.
The team developed a series of aptamers that recognise different growth factors, and anchored one end of each aptamer to a collagen substrate. To the other, they attached a cell-adhesive peptide that a target cell type could recognise, grab on to and pull. When the cell applied traction forces, the aptamer unravelled and its growth factor cargo was released. The team calls their invention traction force activated payloads (Traps).
‘It is the first example of an engineered system that uses traction forces to release a therapeutic,’ Almquist says. ‘We showed if you change the handle on the aptamer to something only certain cells recognise, you can make it so different cells can release different proteins.’ The team is now looking at ways to use Traps to start to direct cell behaviour. ‘There are time courses in wound healing where certain cells arrive and others leave. Now we can design materials where, give or take a little bit of time, those signals will be activated whenever the right cell is present.’
As synthetic constructs, it is not just the cell-binding end of the Trap that can be altered. They can be anchored to many different substrate materials. ‘We are looking at things like 3D printing them, to spatially pattern in three dimensions different Traps that have different molecules attached.’ By controlling not only temporal but spatial growth factor release, the printed matrix could direct cells in certain regions where to go.
One possibility is that the Traps can be used to help orchestrate the coming and going of different immune cell types that are key to different phases of wound repair. ‘There is a lot of interest in how we can use the immune system to modulate wound repair,’ Almquist says. ‘If you look at regenerating organisms like salamanders, they always have immune cells in there conducting the process.’ By inducing certain immune cell types to arrive earlier or leave faster, it might be possible to start to shape wound repair and reduce scarring.
Initially, being able to influence immune cell arrival and departure during wound repair would be a useful research tool for understanding wound healing processes in more detail and how it might be shaped. And any insights that do come from this work should be directly translatable into clinical use. ‘One of the motivations for basing the platform on aptamers is there are clinically approved aptamers – so there is a pathway, an ecosystem for making these and getting them into the clinic,’ says Almquist.
‘Going into the fourth dimension, designing these dynamic systems that can respond bidirectionally over time with a tissue – this really seems to be the next generation of biomaterials,’ Almquist says.
James Mitchell Crow is a science writer based in Melbourne, Australia
References
1 A Matsumoto et al, Sci. Adv., 2017, 3, eaaq0723 (DOI: 10.1126/sciadv.aaq0723)
2 S Chen et al, ACS Biomater. Sci. Eng., 2019, 5, 5781 (DOI: 10.1021/acsbiomaterials.9b00532)
3 B P Purcell et al, Nat. Mater., 2014, 13, 653 (DOI: 10.1038/nmat3922)
4 B A Badeau et al, Nat. Chem., 2018, 10, 251 (DOI: 10.1038/nchem.2917)
5 P M Gawade et al, Adv. Mater., 2019, 31, 1902462 (DOI: 10.1002/adma.201902462)
6 A Stejskalová et al, Adv. Mater., 2019, 31, 1806380 (DOI: 10.1002/adma.201806380)













No comments yet