Cannabinoids are finally coming out of the shadows and onto the shelves of pharmacies around the globe. Rachel Brazil reports
In August 2013, US TV documentary Weed highlighted the case of Charlotte Figi, a six-year-old with Dravet syndrome. This rare, uncontrolled epilepsy caused her to have over 300 seizures a week, as well as severe cognitive and motor delays. After all other treatments failed, and with the support of her neurologist, Figi’s parents decided to treat her with oil extracted from the cannabis plant, which has been legal for medicinal use in Colorado, where the family live, since 2000. The seizures drastically reduced and after eight months she was 99% seizure free. In addition, according to her mother, Figi’s severe autism-like behaviours have also gone.
The type of cannabis used to treat her had been cultivated to be extremely low in tetrahydrocannabinol (THC) the psychoactive component of the plant, but high in the molecule cannabidiol (CBD). The strain, named Charlotte’s Web after Figi, was developed by the Stanley family. This family set up a foundation called Realm of Caring that supplies marijuana to patients, some of whom have relocated to Colorado from states where its use is not permitted, giving rise to the term ‘marijuana refugee’.
Almost as significant as Figi’s story was the public apology of the documentary’s presenter and celebrity doctor Sanjay Gupta. He said this case had made him reassess the evidence on the medical use of marijuana and he apologised for previously opposing its legalisation. He catalogued the many other areas where there are indications of its value: pain relief, inflammatory conditions and even slowing tumour growth. The media coverage, coupled with campaigning from parents like Figi’s, had a huge impact in the US. Since 2013, a further five states have passed laws, giving a total of 23 states where medical marijuana is now permitted under state laws.
Creating drugs from drugs
In the UK, the legal status of marijuana was revisited in August 2014, when then drugs minister, Norman Baker, called for a review of its medicinal properties, amid concerns that credible people were having to break the law to treat their conditions. The Department of Health stated it had no plans to change the law. Perhaps one reason for this is because of Salisbury-based GW Pharmaceuticals’ progress in developing medicines from cannabis. In 1998 they were given a licence to work in this area, and in 2011 their first drug Sativex was approved in the UK for treating multiple sclerosis muscle spasms. It is now approved for treating this condition in 23 countries. The mouth spray, containing both THC and CBD extracts is also being tested for cancer pain management. A second product, Epidiolex, is a pure CBD extract and is in clinical trials for the treatment of Dravet syndrome, the type of epilepsy suffered by Figi. Clinical trials using combinations of THC and CBD extracts for treating inflammatory bowel disease, brain cancer and diabetes are also underway.
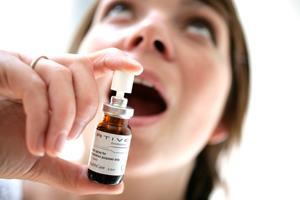
The company already has some indication of Epidiolex’s performance. In October 2014, they announced results from an ‘expanded access’ programme whereby a small number of US neurologists were allowed to prescribe the drug. Overall 40% of patients had their seizure frequency at least halved, with 5% becoming altogether seizure free. Whilst not controlled trials, these figures are impressive given that the patients involved had failed to respond to other drugs and GW Pharmaceuticals are hopeful that Epidiolex will be licensed for treating Dravet syndrome by 2017.
Creating pharmaceutical-grade medicines from cannabis is a tricky business, explains Stephen Wright, GW Pharmaceuticals’ R&D director. In an undisclosed location, the company cultivates 200 tonnes of cannabis flowers each year, cloned from a number of cross-bred plants and grown in carefully regulated greenhouses to create a standardised product. Wright explains that because they are growing a controlled substance, ‘we are subject to regular inspections [and] everything we do is indoors, under glass, with security’.
The endocannabinoid system
The medicinal use of cannabis goes back five millennia and it is often said that Queen Victoria’s doctor John Russell Reynolds prescribed it for her menstrual cramps (although he was certainly a proponent, there is no evidence of this). Our current understanding of cannabis pharmacology stems from the 1964 work of the Israeli chemist Raphael Mechoulam. Mechoulam, who has been at the Hebrew University in Jerusalem since 1966, characterised the structure of THC and later identified the body’s own cannabinoids; anandamide and 2-arachidonoylglycerol. These molecules, their receptors and related enzymes, discovered in the early 1990s, make up the endocannabinoid system.
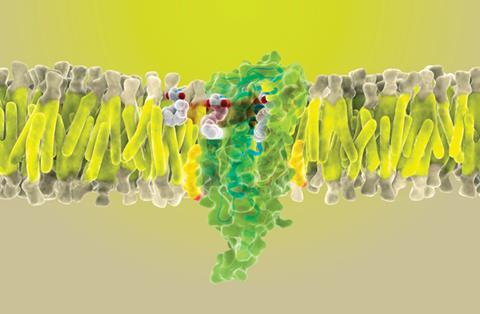
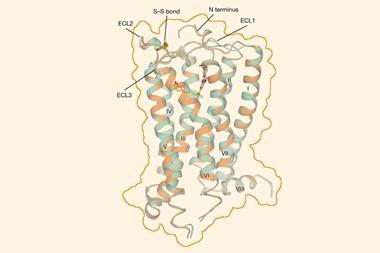
In 1998, leading cannabis researcher Vincenzo Di Marzo from the Institute of Biomolecular Chemistry in Naples, Italy, described the endocannabinoid system’s purpose as allowing our bodies to ‘relax, eat, sleep, forget and protect’. Via two cannabinoid receptor proteins, CB1 and CB2, the endocannabinoid system regulates the release and re-uptake of a range of neurotransmitters, acting as a neurotransmission thermostat for the central nervous system, immune system, gastrointestinal tract, reproductive system, cardiovascular system and endocrine network. CB1 receptors are found mostly in the brain and CB2 in the immune system, both functioning in parallel with other systems. The euphoric high feeling and therapeutic effects that THC induce can be explained through its binding to CB1 receptors, which causes increased neurotransmitter levels by stopping the re-uptake of these molecules.
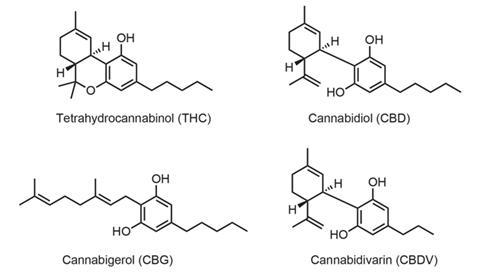
But the pharmacology of cannabis is more complex than THC alone. Ben Whalley, a professor of neuropharmacology at the University of Reading, UK, explains that as well as THC, small amounts of another 107 terpenophenol cannabinoids have been extracted and identified from the glandular hairs on the female flower of the Cannabis sativa plant. These include CBD, its biosynthetic precursor cannabigerol (CBG), and another derivative, cannabidivarin (CBDV). Cannabis is the only plant known to contain these compounds and Whalley says they probably act as a built-in insect repellent. Today, most street cannabis has been bred to maximise THC content: that can account for up to 25% of the dry cannabis flower’s weight. The flower also contains an additional 200 aromatic terpenoids. ‘The pungent odour that people smell when someone walks past smoking a joint is actually all of those terpenoids,’ says Whalley.
The entourage effect
Whilst synthetic THC has been available since the mid-1980s as dronabinol for treating Aids related weight loss and chemotherapy symptoms, it was not always well tolerated by patients who often report that its psychotropic side effects are greater than those of botanical cannabis. This is partly because ingested THC is metabolised by the enzymes in the stomach and gut into the 11-hydroxy-THC form, which has a more potent and prolonged effect. But another explanation is the absence of other cannabinoids, such as CBD, present in the plant and the drug Sativex. In fact, when THC is combined with CBD, there is a therapeutic benefit and a decrease in the adverse effects of THC alone and this has been exploited in Sativex, where purified THC and CBD extracts are mixed equally.
The phenomenon was labelled ‘the entourage effect’ by Mechoulam. He suggested that the plant cannabinoids were working in synergy in a similar way to mechanisms occurring in the body’s endocannabinoid system. Here, fatty-acid derived modifier molecules are released with the natural cannabinoids providing a protective cushion and preventing their recapture by cells, meaning they can continue to target cannabinoid receptors. A similar process could explain why CBD improves the drug-performance of THC, and other cannabinoids that may work synergistically.
During a presentation at a GW Pharmaceuticals R&D day in October 2014, Di Marzo stated that ‘there is already pre-clinical data showing that a THC-CBD combination is more effective in reducing glioma [brain tumour] cell growth and there is similar data for the combination of CBD and CBG in other types of cancer’. GW Pharmaceuticals are now carrying out early clinical safety trials for treating glioblastoma multiforme, an aggressive kind of brain tumour. Low doses of THC and CBD added to standard chemotherapy drug temozolomide show increased survival times in animal tests.
CBD and schizophrenia
Perhaps the last condition you would think cannabis would have therapeutic value for is schizophrenia. In 2009, the UK government rescheduled the drug to the higher class B category, citing research linking heavy use of high THC strains to the onset of schizophrenia in vulnerable young people. But it turns out that CBD has the opposite effect. Neurologist and psychiatrist, Markus Leweke from the Central Institute of Mental Health in Mannheim, Germany, carried out several clinical trials, which showed CBD had comparable antipsychotic effects to currently used medication and was better tolerated. GW Pharmaceuticals have also started schizophrenia clinical trials with their purified CBD extract. Leweke says ‘it’s fairly clear that we see a malfunction or a disturbance of the endocannabinoid system in patients with schizophrenia.’
Understanding why CBD has this effect is not straightforward, because CBD does not directly interact with either the CB1 or CB2 receptors. Leweke says he is ‘pretty sure that the relevant mechanism is the increase in anandamide’. He has shown that higher levels of this natural cannabinoid in schizophrenic patients corresponded to a reduction in psychotic symptoms. The hypothesis is that CBD inhibits the enzyme FAAH (fatty acid amide hydrolase) responsible for breaking down anandamide. This then causes more activation of CB1 receptors to balance neurotransmission in the brain and suppress psychotic symptoms.
Whalley doesn’t, however, think that this is how CBD works for treating epilepsy and says ‘there is no real evidence that suggests that CBD interacts with the endocannabinoid system’. Understanding the antiseizure mechanism of CBD and CBDV, another cannabinoid with a good antiseizure profile, is now a priority for his research group.
He predicts that understanding how CBD works will also enable the development of superior synthetic drugs that mimic its action. ‘At the moment there is nothing to say that CBD or CBDV are in any way optimised, so you might be at relatively low potency for a target that we haven’t yet properly identified. We are poking around the dark a little bit, doing phenomenological rather than target-based, empirically driven drug development.’
A return to polypharmacology
But Di Marzo instead thinks that plant cannabinoids offer a different approach to drug development and a return to milder, multi-target drugs. Conventionally, this is seen as something to avoid in order to reduce drug side effects. When presenting in October, Di Marzo explained his perspective: ‘rather than developing compounds, the so-called magic bullets that activate one single target very potently, we can go back to the old concept of polypharmacology and try to target more than one target with lower potency’. The therapeutic profiles of many cannabinoids show moderate interactions with multiple drug targets, each having its own distinct pharmacological fingerprint.

Di Marzo argues that an unbalancing of the body’s natural systems causes disease – for example, too much cell death leads to neurodegenerative diseases or not enough leads to cancer, too much neurotransmission leads to epilepsy or not enough leads to Alzheimer’s disease. However, with cannabinoids the body seems to recruit its own endocannabinoid control system. Possibly working via multiple targets, cannabinoids can both activate and reduce over-stimulation to restore balance. So plant cannabinoids may present a polypharmacological solution, he claimed, without the side effects of high potency drugs. The multi-target, rebalancing properties of cannabinoids also explains why they show promise as drugs in such a wide variety of conditions.
Campaigns for legalisation
Whilst cannabis itself remains illegal in the UK, cases like that of Figi only add to the conviction of those campaigning for its legalisation for medical use. Keiron Reeves from Sussex is a member of the UK medicinal cannabis use campaign group, the United Patients Alliance, and has had epilepsy since childhood. Conventional medication did not help and after suffering a seizure whilst cycling in traffic, he decided to go to Amsterdam, where cannabis is legally available, and try cannabis oil. He says it has changed his life and he now finds his own supply in the UK. ‘I’ve only had three seizures in the last 18 months. That is a complete success story for me, because I was having them every other week.’ Reeves estimates at least 15,000 patients use cannabis medicinally in the UK, including people with late-stage cancer and multiple sclerosis. Although Sativex is licensed to treat multiple sclerosis, he says most sufferers find it impossible to get it prescribed on the NHS due to ‘a post code lottery’. Whilst the Welsh government have chosen to fund it, currently the National Institute for Health and Clinical Excellence (Nice) and the Scottish Medicines Consortium (SMC) have ruled that it is not cost effective.
In the US, the Epilepsy Foundation has come out in support of the rights of patients living with uncontrolled epilepsy to access medical marijuana, if the potential benefits outweigh the risks. The legal situation in the US is complicated however, because even though state laws in 23 states permit some medical use of cannabis, the Federal government still classes it as a Schedule 1 drug, meaning it has ‘no currently accepted medical use’. This legal confusion makes it difficult for patients to know their legal rights, and for researchers to carry out scientific research and run clinical trials. In the UK, medical charities seem to be taking a more cautious approach. The UK’s Epilepsy Society says that the topic is discussed on their forums, but they are not advocating any legal changes at present.
Stephen Wright says GW Pharmaceuticals has no position on the legality of medical marijuana, but that it ‘illustrates an issue that repeatedly occurs, which is if something appears to work should people be able to use it and should it be called a medicine or should a medicine be something which has been through a whole raft of studies to determine efficacy and safety’. Cannabis he sees as ‘outside of the normal remit of the way medicine is practised’, like the great number of other alternative therapies that many patients use, alongside conventional medicine. But, says Wright, in time, as we fully exploit the medicinal properties of cannabinoids, the issue might just go away. ‘Opioids are widely used in pain relief on prescription in hospitals and nobody says, actually I’d rather smoke opium.’
Rachel Brazil is a science writer based in London, UK
Further reading
Weed documentary: https://www.youtube.com/watch?v=hrVXRZY1_x0












No comments yet