Can peptide hormone mimics avoid the side effect pitfalls of previous weight loss treatments?
A new class of drugs for obesity, which suppress appetite by mimicking human hormones, are being developed by the pharmaceutical industry in its latest effort to access the lucrative potential market for weight loss treatments.
Eli Lilly’s Mounjaro (tirzepatide) was approved for treating diabetes in the US, Canada and Europe in 2022, and brought in sales of almost $500 million (£400 million) last year. The company is now seeking approval from US and European regulators to extend the drug’s use to obesity treatment, with decisions expected as soon as late 2023. This could propel tirzepatide towards $50 billion in peak sales according to some market analysts, making it the best-selling drug ever.
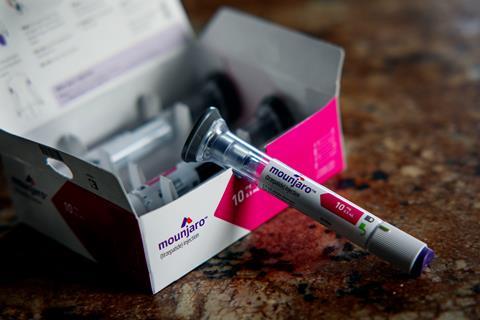
The drug is similar to Novo Nordisk’s semaglutide, marketed as Ozempic for diabetes since 2017, but also approved for weight loss (as Wegovy) by the US Food and Drug Administration (FDA) in 2021, and European Medicines Agency (EMA) in 2022. In March this year, the UK’s National Institute for Health and Care Excellence (Nice) recommended its use for managing obesity. Estimates suggest it could produce sales of $3–4 billion in the US alone this year.
GLP-1s are normally stimulated in the intestine. They act on the brain to tell us we are full and to decrease appetite
Both drugs are injectable peptides that mimic a natural hormone, glucagon-like peptide-1 (GLP-1). Semaglutide differs from natural GLP-1 in just two amino acids, but that slows its degradation in the body from hours to days. The first GLP-1 mimic was AstraZeneca’s Byetta (exenatide), originally isolated from the venom of Gila monster lizards. It was first approved in 2005 for diabetes, injected twice daily.
Feeling fuller
‘GLP-1s are normally stimulated in the intestine. They act on the brain to tell us we are full and to decrease appetite,’ says Fatima Cody Stanford, an obesity physician at Massachusetts General Hospital and Harvard Medical School, US. In 2020, Nice in the UK recommended its first GLP-1 agonist, liraglutide (Saxenda, Victoza) from Novo Nordisk, for managing weight and obesity, alongside diet and physical activity.
The GLP-1 mimics work by decreasing food intake and by increasing secretion of insulin, the hormone that reduces blood sugar. They also slow stomach emptying and stymy production of glucagon, a hormone that raises blood glucose levels. Another effect, says Stanford, is to convert white fat to brown fat tissue, which burns more energy at rest.
For semaglutide, the Step-1 clinical trial showed on average 15% weight loss in people with obesity who injected it weekly for 68 weeks, along with lifestyle changes. In Lilly’s Surmount-1 and Surmount-2 trials, adults receiving tirzepatide once weekly showed average weight loss of 15–21%, depending on dose, compared to 3% for those receiving a placebo.
While tirzepatide is yet to be approved for weight loss, it is attracting attention because it also mimics another hormone, glucose-dependent insulinotropic polypeptide (GIP). This regulates energy balance via a receptor in brain and fat tissue. ‘This is an even more interesting compound,’ says obesity researcher John Speakman at the University of Aberdeen, UK. ‘Lilly produced a drug that is a combination of a GLP analogue and a GIP analogue, which breaks apart in the system and hits both receptors.’ There are indications that the dual approach is synergistic.
An escalating global issue
New results and praise from celebrities have pushed obesity drugs into the headlines. But weight loss is not just a goal of the rich and famous. ‘The dramatic rise in obesity in the past few decades started in some high-income countries, but it is really affecting low- and middle-income countries now,’ says Louise Baur, a childhood obesity researcher at the University of Sydney in Australia.
The World Obesity Federation predicts that most of the global population – over 4 billion people – will be overweight by 2035 on current trends. The World Obesity Atlas 2023 warned that lower-middle income countries such as India, Pakistan, Indonesia and Nigeria might follow the pattern of upper-middle income countries such as Mexico, Brazil and Turkey in seeing rapid spikes in obesity, especially for children and adolescents.
It is not as if the whole world decided to become gluttonous and slothful. People respond physiologically to a pathological environment
The federation predicts 47% of Mexicans, 46% of South Africans and 42% of Malaysians will be living with obesity by 2035. ‘You’ve started to see rises in the Middle East, in South America and countries such as China and Thailand,’ says Baur. This occurs especially as communities become more sedentary and switch from a more plant-based diet to more processed foods. ‘It is not as if the whole world decided to become gluttonous and slothful. People respond physiologically to what is a pathological environment,’ says Baur. ‘Humans are evolved to like food and not be unduly active.’ Processed foods and everyday obesogenic chemicals are also increasingly implicated in triggering weight gain.
Obesity experts point to the abject failure of advice to improve nutrition and activity levels and interventions aimed at lifestyle to tackle the obesity epidemic. ‘None of our countries do a good job,’ says Stanford, who says that between 5 and 7% of people respond to lifestyle changes alone. She says that effective pharmaceutical interventions offer much-needed additional treatment options.
Avoiding past failures
The past landscape of weight loss drugs is littered with failures, however. Some failed during clinical trials, while others were withdrawn after regulatory approval. A 2016 study detailed 47 obesity drugs withdrawn because of adverse drug reactions, mostly due to heart problems, addiction issues or psychiatric effects.
One of the first weight loss drugs was metabolism-accelerating 2-4-dinitrophenol, recognised when exposed factory workers lost weight. It was banned in the late 1930s after numerous deaths and severe side effects. Amphetamines were subsequently popular and included in rainbow diet pill concoctions, which caused dozens of deaths up to the 1960s and sporadically reemerged, with the FDA warning in 2012 about supplements with multiple agents.
More recently, rimonabant (developed by Sanofi-Aventis) was approved as a cannabinoid receptor blocker in Europe in 2006, but was removed two years later after serious psychiatric side effects emerged. Meanwhile, sibutramine (Meridia from Abbot Laboratories) became popular after FDA approval in 1997, until it was linked to heart problems and strokes and withdrawn in Europe and the US in 2010. The drug suppresses appetite by blocking serotonin and noradrenaline from being taken back up after acting as neurotransmitters in the brain. In 2020, eight years after its approval, the FDA withdrew Belviq (lorcaserin) after a trial showed increased cancer risks. Lorcaserin reduces appetite by activating a serotonin receptor in the hypothalamus.
Anti-obesity medicines aren’t the answer to everyone’s obesity – some people don’t need them
Qsymia, a combination treatment consisting of phentermine and topiramate, remains available in the US, but was refused European approval owing to cardiovascular concerns and psychiatric and cognitive effects. There are sound biological reasons for issues with some of these drugs, says Speakman. ‘Fat storage, the amount we eat and the energy we expend are all regulated in the hypothalamus. That area of the brain regulates a lot of other things, so there is great potential for side effects once you start fiddling around there [with drugs].’
Orlistat (GSK’s Alli, Xenical) represents another approach to weight loss, remaining in the gut and blocking enzymes there that digest fat. ‘It works on the old premise that people with obesity must eat a lot of fat,’ says Stanford, who typically does not prescribe it due to its low efficacy. It stops about a third of fats you eat from being absorbed by the body, generating more gas and oily poo that can produce off-putting effects. ‘You get this delightful phenomenon called anal leakage,’ says Speakman.
Balancing benefits with side effects
The newer GLP-1 mimics also bring their own downsides, sometimes lost in hype. The most common for semaglutide are nausea, stomach pain, constipation, diarrhea and vomiting. ‘Nausea is hands down the number one side effect, impacting about 45% of people,’ says Stanford. ‘Side effects are typically transient. If they are persistent then that’s not the right drug for that person,’ she adds.
The common side effects for tirzepatide are similar. Speakman says around 20% of patients experience nausea, for example. ‘It is thought that the second agonist, GIP, makes its tolerability profile relatively better,’ says Evan Seigerman, a biotech market analyst at BMO Capital Markets.
Another drawback is that people start to regain weight once they stop taking GLP-1 drugs. This suggests that people may require injections for long periods, possibly for life. Nice has recommended semaglutide be used for a maximum of two years. Many expect that guidance to change as more safety data becomes available. Right now, the drug is expensive for long-term use. Some health insurers in the US will cover the cost, but others will not – for example the government-funded Medicare programme for over-65s does not cover weight-loss medications.
What could transform the picture is evidence for bonus health benefits. The Select trial is examining the impact of semaglutide on heart disease and stroke in patients who are overweight or obese. Results may become available over the next few months, says Seigerman. There is some previous evidence for GLP-1s used to treat type 2 diabetes moderately reducing major cardiovascular events and all-cause mortality.
Stanford is optimistic. ‘GLP-1s are normally produced in the body, mostly in the GI tract, but they protect our brain and increase cardiac output,’ she says. ‘We see a decrease in all-cause mortality, and fatal and nonfatal strokes and heart attacks,’ she says. ‘We haven’t seen this previously with more traditional agents used for weight regulation.’
Scope for competition
Faced with an obesity epidemic, an effective pharmaceutical intervention seems sure to remain in high demand. Novo Nordisk has restricted supplies of lower dose semaglutide injectors to limit the number of new patients starting on the drug until it can ramp up manufacturing capacity.
The potential market is large and lucrative. ‘I don’t think anti-obesity medicines are the answer to everyone’s obesity – some people don’t need them,’ says Stanford. ‘But we are woefully undertreating this disease.’ This leaves plenty of scope for other drugs for a disease linked to dozens of other debilitating conditions.
Altimmune has completed a phase 1 trial of a peptide-based agonist, Pemvidutide, that activates GLP-1 and glucagon receptors. Amgen has begun a phase 2 trial of AMG133, which targets both GLP-1 and a protein responsible for boosting glucose-dependent insulin production. And Lilly has also developed and run a small study on a triple glucagon, GIP and GLP-1 receptor agonist.
Meanwhile, Pfizer reported on a small molecule oral agonist of GLP-1 receptors, and carried out a phase I study in Japanese adults with type 2 diabetes. ‘There’s a lot of new small molecules in development that could potentially be used as maintenance therapy [after an injected GLP-1 mimic],’ says Seigerman. Baur welcomes the fact that multiple related drugs are heading towards market, adding ‘competition does marvels for cost.’ There is hope that this new class of drug will deliver health benefits without too many serious side effects. ‘Most people in the obesity field feel that these are very good drugs,’ says Speakman. ‘It feels like we’ve really turned a corner in terms of obesity pharmacology.’















No comments yet