Ben Valsler
Happy New Year! If you, like so many others, have resolved to lose weight in 2017, then as well as running shoes, gym membership and calorie counting apps, you may have considered getting some chemical help. This week, Kit Chapman looks at a ‘poster child’ in the battle against obesity…
Kit Chapman
In 2010, the anti-obesity drug sibutramine was suspended from use throughout Europe by the European Medicines Agency. After a long review, it had ruled that its risks – particularly of stroke and heart attack – were greater than the benefits. Abbot Laboratories, the drug’s maker, also withdrew it from sale. The move left only one prescription drug on the market to help weight loss: orlistat.
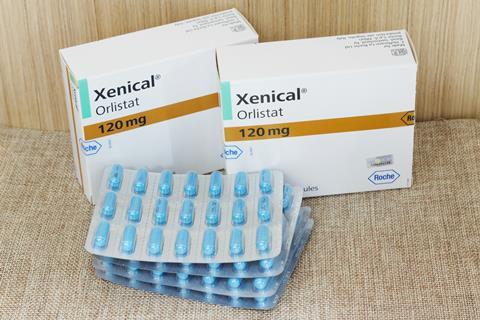
Orlistat is arguably a poster child of the battle against obesity. While weights bulge around the world, the drug, first launched in 1999, has been prescribed to some 40 million people to help weight loss in conjunction with a reduced calorie diet. The secret to its success is probably its relative safety. While the drug can have serious side effects, such as liver damage, these are few and far between. This has made the drug available over the counter in several of the biggest weight loss markets in the world, such as the US, UK and Australia, under the names Xenical or Alli.
The lack of side effects is largely down to how orlistat works. While most drugs work systemically – they are absorbed by the body – orlistat largely remains in the gastrointestinal tract before it’s excreted in poo. The good news is that this is exactly where it needs to be to get to work. The drug’s mechanism of action is to bind to lipases, enzymes that break down triglycerides in the intestine, meaning that they aren’t absorbed by the body either. At a standard prescription dose, orlistat prevents around 30% of fat being absorbed, while over the counter doses typically prevent around 25%. All this means that, with the help of a smart diet, fat is cut down and the patient loses weight.

There is a catch, though. As you might have guessed, if the fat isn’t being absorbed by the body, it has to go somewhere – and non-absorbed fat really isn’t very pleasant. The drug says there’s no real side effects if you eat less than 15g of fat in a meal. Go over this limit, though, and expect streatorrhoea – oily, loose stools – accompanied by flatulence, urgent bowel movements and possible incontinence. All of this gets worse the more fat you eat, meaning that orlistat isn’t an excuse to tuck in to your favourite fatty treats.
This may not sound pleasant, but for obese patients it’s a definite weight loss option. And, if it’s part of a healthy, low-fat diet, it’s proven to cut down weight and reduce the risk of conditions such as cardiovascular disease and diabetes.
Like any drug, orlistat is a tool that, when used correctly, makes a difference. You just really don’t want to use it then go out for a curry.
Ben Valsler
Kit Chapman there on orlistat, and the unpleasant side effects you may experience if you forget to watch your fat intake while taking it. Next week, Matt Gunther brings us the story of dioxin, and one of the largest environmental disasters in European history.
Matt Gunther
At the time of the release, authorities didn’t really know how the chemical, a contaminant also found in the infamous wartime defoliant ‘Agent Orange’, would affect the surrounding population. They would soon find out.
Ben Valsler
Join Matt for that rather grim story next week.
Now, eagle-eyed (or should that be bat-eared?) listeners may have noticed a small mistake in our diborane podcast a few weeks ago – many thanks to Alix Harrow who emailed to point it out. We’ve fixed the slip up now, but if you spot anything else we’ve missed, or would like to suggest a compound for us to cover, then please do get in touch – email chemistryworld@rsc.org or tweet @ChemistryWorld. I’m Ben Valsler, thanks for joining me.












No comments yet