Ben Valsler
This week, Kat Arney introduces a powerful cancer drug that stops tumours from developing and spreading by preventing one of the fundamental processes of cell division…
Kat Arney
Fluorouracil, or 5-FU, is a powerful drug in the chemotherapy arsenal, used to treat breast, stomach, bowel and other types of cancer. And although it’s widely used today – and is on the World Health Organisation’s List of Essential Medicines, which should be included in even the most basic healthcare systems – its origins lie back only in the 1950s.

When the structure of DNA was discovered in 1953 by James Watson and Francis Crick, with help from Maurice Wilkins and Rosalind Franklin, it was known that it was made up of repeating molecular subunits, strung together and twisted into the famous double helix. These subunits are nucleotides, each consisting of a sugar (deoxyribose), a phosphate group, and a compound known as a base. There are four bases – adenine, cytosine, thymine and guanine – usually referred to by their initials A, C, T and G. Two of these – A and G – are made up of two rings of carbon and nitrogen, and called purines, while T and C are single rings, known as pyrimidines. There’s also another type of pyrimidine called uracil, or U, which is found in RNA – a biological messenger molecule that is very similar to DNA. Incidentally, a handy way to remember which bases are purines is that A and G make up the chemical symbol for silver, and if you imagine a silver soup tureen, then that rhymes with purine. Well, it works for me…
Because purines and pyrimidines are the main components of DNA, they are absolutely fundamental to life. Without them, cells can’t make new copies of their DNA in order to divide. Cancer cells multiply much faster than most healthy cells, so they have a tremendous hunger for purines and pyrimidines. In 1954, researchers Abraham Cantarow and Karl Paschkis found that liver cancer cells took up radioactive uracil much more easily than normal liver cells. Cancer cells tend to put uracil into their DNA, even though it shouldn’t normally belong there, only in RNA.
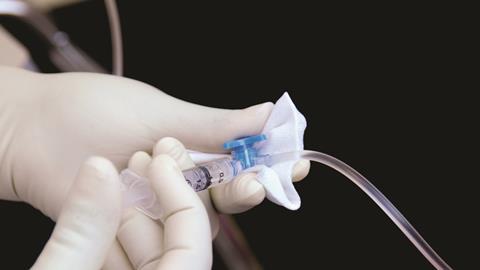
At the same time another scientist, Charles Heidelberger, was investigating how chemicals containing fluorine could bind to important proteins in cells and stop them from working. So he asked chemists at the company Hoffman-La Roche to make a version of uracil containing fluorine – fluorouracil, or 5-FU. When he tested it in mice, Heidelberger was pleased to find that his new drug had a potent anti-cancer effect, publishing his findings in the journal Nature in 1957. Clinical trials followed throughout the 1960s and 70s, working out how best to give fluorouracil and what doses to use. One problem is that the drug needs to be given continuously, because it is quickly broken down in the body. This only really became possible in the 1970s with the development of intravenous drug delivery pumps that patients could carry around with them.
Fluorouracil mainly works by blocking an enzyme called thymidylate synthase, which performs one of the steps in the process of making thymine in cells from a uracil-like precursor. With this enzyme shut down, cells quickly run out of thymine, meaning they can no longer make new DNA. And if they can’t make new DNA they can’t multiply, so they die.
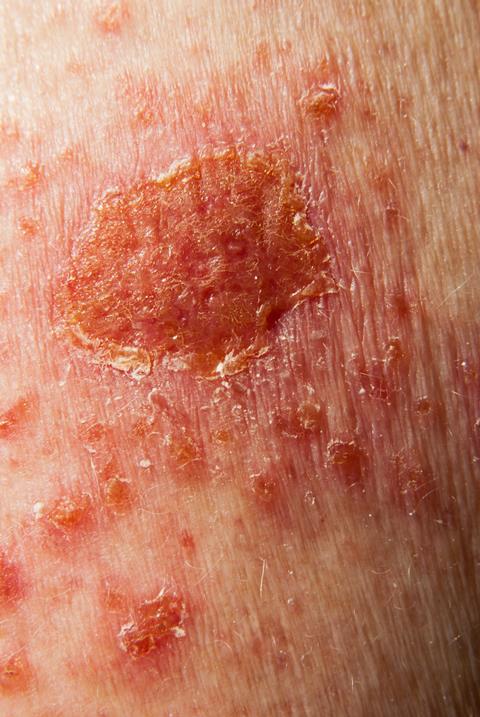
This way of working puts fluorouracil in the class of drugs known as anti-metabolites – they look similar to chemicals found normally in cells, but instead block the fundamental manufacturing reactions that help to keep cells alive. But it’s not just cancer cells that need to make new DNA – healthy cells do too, and the drug also affects them. Because of this, fluorouracil can have some pretty unpleasant side effects, including suppressing the immune system and increasing the risk of infections, anaemia due to a drop in red blood cell production, hair thinning, bruising and more. Women taking fluorouracil are also warned not to get pregnant, because the drug will also stop the production of DNA in the dividing cells of a growing foetus.
Today, researchers are working on developing and testing chemically tweaked versions of fluorouracil, with different properties. For example, capecitabine, also known as Xeloda, is what’s known as a prodrug. On its own it doesn’t have an effect, but it’s broken down by enzymes in the body to produce fluorouracil. Having a range of versions means that there are more chances of finding the right drug for the right patient, taking a more personalised approach to cancer treatment.
Ben Valsler
Kat Arney on fluorouracil, one of many drugs used to treat cancer. Kat will be back with another DNA-disrupting compound soon. Next week, another Kat – this time Katrina Kramer – on the vital role of chemical companions…
Katrina Kramer
Every hero needs a sidekick. Think Batman and Robin, Shrek and Donkey, or, if you prefer something more classic, Don Quixote and Sancho Panza. In organic chemistry, if metal catalysts are the heroes, ligands are their sidekick.
Ben Valsler
Katrina examines a versatile and extremely useful catalyst in next week’s Chemistry in its Element podcast. Until then, please get in touch with any compounds you’d like to hear more about – email chemistryworld@rsc.org or tweet @chemistryworld. I’m Ben Valsler, thanks for listening.










No comments yet