Cone snails deploy sophisticated venom cocktails to paralyse prey. Anthony King talks to the researchers harnessing these peptides to develop new pain medications
- Cone snail venoms contain vast libraries of potent, structurally robust peptides that target ion channels and receptors, offering a rich but largely untapped source of potential pain‑relief drugs.
- Only one cone‑snail‑derived drug, ziconotide, is currently approved, and its need for spinal delivery highlights the major challenge of safely and effectively delivering venom peptides.
- Recent advances – including stabilised peptide designs, GLP‑1–inspired delivery breakthroughs, and new insights into conotoxins targeting GPCRs, sodium channels and inflammation pathways – are renewing interest in venom‑derived analgesics.
- Researchers argue that pain may require multi‑target approaches, echoing the synergistic action of natural venoms; emerging tools in peptide engineering and genomics are fuelling cautious optimism despite past setbacks in clinical translation.
This summary was generated by AI and checked by a human editor
There’s a mottled pinkish-white snail hiding at the bottom of a tropical reef somewhere off eastern Australia. At nighttime, it will target small fish by squirting venom into the water to disorient and slow them down. Then it will fire a hollow harpoon, laden with neurotoxins, that is actually a tethered tooth. Remarkably this 10–15cm geographic cone snail (Conus geographus) contains venom potent enough to kill an adult human.
What’s delivered by its hypodermic-like needle is a sophisticated cocktail of peptides that target ion channels and receptors, triggering paralysis in fish. It inspired the discovery of tens of thousands of biologically active peptides known as conotoxins in dozens of cone snail species, a potential bonanza for drug discovery. ‘They’ve 250 or more compounds in their arsenal. I’d describe it as a cluster bomb because it fans out to hit as many things as possible,’ says Mandë Holford, a chemist and marine venom investigator at Harvard University in Boston, US. Most of these venom constituents remain uncharacterised.
Holford’s lab and others focus on identifying venom peptides that could have therapeutic uses. ‘The venom arsenal is extremely compelling from a chemical standpoint. It’s made of this immense cocktail of compounds with physiological properties,’ says Holford. ‘We’re finding out that what kills you can also cure you.’ As yet, however, few of these peptides have benefited patients.
The ziconotide breakthrough
Some venom peptides from cone snails block pain in the fish, presumably to stop them darting away – which is essential if you are a snail. ‘They don’t just paralyse the fish. They hit multiple targets in the prey,’ says Helena Safavi, marine venom researcher at the University of Utah, US. Safavi is a biologist who first fell in love with scuba diving in a chilly lake in her native Germany, before doing a postdoc in biochemistry in Australia and a stint in Denmark.
![]()
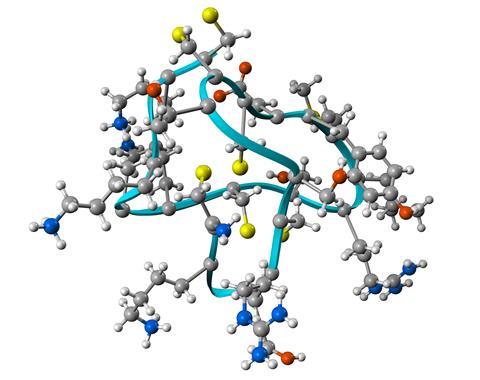
She now studies marine venom from her lab in landlocked Utah, which is where biologist Baldomero Olivera pioneered snail venom research and helped develop the drug ziconotide (Prialt) for chronic pain. This synthetic version of a snail peptide blocks N-type calcium channels on nerve cells in the spinal cord. Conotoxins usually consist of 10 to 30 amino acids and are often exquisitely shaped for a receptor, making them effective ligands. Prialt has been estimated at 1000 times more potent than morphine. Unlike morphine and other opioids, however, it is not addictive. Yet it comes with a downside: it must be delivered directly to the spinal fluid via a special pump and its use is restricted to severe intractable pain. Peptides cannot cross the blood–brain barrier and are broken down in the low pH of the stomach and digested by enzymes. Delivery is a pitfall that has weighed on other efforts to convert the marine venom pharmacopeia into drugs.
Venom aficionados see a light ahead, however, kindled by GLP-1 drugs becoming a billion-dollar industry based on injected peptides inspired by lizard venom. The natural compound from lizards is easily metabolised, so huge efforts went into improving the persistence of GLP-1 analogues for diabetes and obesity treatments. Developers swapped in amino acids targeted by enzymes and bolted on non-natural amino acids such as 2-aminoisobutyric acid. But many conotoxins have a head start in being remarkably robust, sporting covalent bonds between cysteine amino acids. Often at least one disulfide bond loops through two others, forming a knot-like structure that is thermally and chemically stable.
This sort of configuration is attracting interest. ‘There’s been an uptick in people developing libraries of disulfide-rich cyclic peptides as starting points for hit discovery,’ says Andrew Jamieson, a peptide chemist at the University of Glasgow, UK. Natural venom has other tricks up its sleeve. A synthetic version of the hormone somatostatin – Octreotide, used to treat endocrine tumours and acromegaly – was engineered to include D-phenylalanine, the mirror image of natural L- phenylalanine. Yet Safavi’s lab discovered a somatostatin-targeting peptide in cone snail venom that looked incredibly similar, with a minimised motif and a D amino acid, which is highly unusual in nature.

Drug developers can start with a venom peptide evolved to be robust, though they usually need to be modified and an injection may still be the most effective delivery route. Nevertheless, the recent example of millions of people self-injecting GLP-1 drugs every week has turned certain assumptions on their head. ‘There’s been a long-standing view that injections would never be acceptable. But especially in the pain field patients are telling us that they would be willing to do anything to get relief,’ says Irina Vetter, a pain and venom researcher at the University of Queensland in Australia.
There is a list of painful chronic conditions, such as diabetic neuropathy and shingles nerve pain, with few effective treatment options. ‘Trigeminal neuralgia is a classic neuropathic condition and has been called the suicide disease because it’s so painful and unpredictable,’ says Steven Cohn, a pain physician and researcher at Northwestern University in Illinois, US. If new effective therapies for such terrible conditions could be developed, it is unlikely that such patients would refuse a relieving jab.
Targeting nicotinic receptors for neuropathic pain
At the University of Utah, pain researcher Michael McIntosh had his interest in marine venoms sparked as an undergrad when he purified the Conus magnus peptide that would give rise to ziconotide. More recently he has focused on venom compounds to be delivered peripherally, especially the small alpha-conotoxins (12–20 amino acids) that interact with nicotinic acetylcholine receptors (nAChR). These transmembrane gates allow cations into a cell when unlatched by a ligand. One peptide from the deadly geographic snail (alpha-conotoxin GI) targets a specific subunit of the receptor at the neuromuscular connection, triggering muscle paralysis.
McIntosh has zeroed in on an alpha-conotoxin from a worm-hunting snail that binds to a nicotinic receptor subtype that is widely present on immune cells. This seems to regulate inflammation that is relevant to neuropathic pain. In mammalian cells, the toxin blocks the receptor on immune cells and alters the release of pro-inflammatory cytokines. The action might indirectly prevent chronic pain, he suggests.
Many chemotherapies are toxic to nerves and cancer patients treated with it can end up with nerve damage that inflicts numbness or pain that can persist for months, years or be permanent. High blood sugar in diabetic patients can also damage nerves. If you look at the inflammatory response to nerve injury, there’s an accumulation of macrophages and T cells, explains McIntosh, and those are reduced when we give a peptide derived from the snail compound. ‘We think that it is producing analgesia not by acutely blocking the receptor, but by altering the pathophysiology so that the nerve doesn’t respond in a way that is abnormal and generate a chronic pain signal,’ says McIntosh. He envisions a weekly injection to patients getting chemotherapy so that nerve damage and neuropathy never develop. At the moment they are working in mice to test safety and efficacy.
Many conotoxins target sodium channels. ‘We would know little about neuronal circuits without venom compounds,’ says Holford. Mu-conotoxin from the marble cone (C. marmoreus) blocks the Nav 1.8 channel and was reported to relieve chronic pain almost two decades ago in animal studies. It has been investigated as a potential pain drug yet no marine venom peptide has directly inspired an approved drug that hits sodium channels.
One challenge is that sodium channels are everywhere in the body. ‘They’re still interesting but also slightly frustrating,’ says Vetter. ‘We think they might be important for effective analgesia. Unfortunately, the pore is very well conserved,’ making hitting specific channels and minimising side effects tricky. Tetrodotoxin from pufferfish is deadly because it blocks multiple sodium channels, interfering with nerve signalling throughout the body.
G protein-coupled receptors: the next frontier
There are plenty of other druggable targets. Safavi’s lab in Utah is investigating venom peptides that hit G protein-coupled receptors (GPCRs), a huge family of membrane proteins that transmit signals from outside. They are major targets of drugs, perhaps making up 36% of all approved medicines. ‘GPCRs are easy to drug, but I think we’ve got all the low-hanging fruit,’ says peptide chemist Jamieson. ‘Conotoxins might be an interesting route to those hard targets,’ especially compact cyclic peptides. He describes them as occupying a Goldilocks space between small molecules – often not very selective – and larger biologics like antibodies, which are more expensive to make. Peptides are also small enough not to attract much attention from immune cells.
The fish stays where it is and doesn’t even know it was injected with a load of venom
The Safavi group studied Asprella cone snails that live at depths up to 250m off the Philippines. They observed that one species stung fish with venom and retreated, before striking the same fish again later. The group hypothesised that this strategy allowed the snail to avoid attachment to dangerous prey. They then discovered a diverse set of peptides that mimic somatostatin hormone, which act on the somatostatin receptor 4, itself a GPCR. ‘It is probably inhibiting pain in the fish,’ explains Safavi. ‘The fish stays where it is and doesn’t even know it was injected with a load of venom.’ The chemical diversity of the hormone mimics make them suitable leads for pain, cancer and endocrine disorder therapeutics, the group reported.
People have five different somatostatin receptors in their bodies. Only somatostatin receptor 4 is implicated in pain signalling, which attracted research interest, but the human hormone is not selective. ‘The two limitations are that somatostatin activates all five receptors and it gets chewed up quickly by proteases in the body,’ says Safavi. However, the cone snail peptide only hits the somatostatin receptor 4 (SSTR4) and it has a minimised structure with disulfide bonds and a D amino acid, as previously noted.
Drug companies have tested SSTR4 agonists for neuropathic and inflammatory pain, with Ely Lilly taking a small molecule (CNTX-0290) into late phase 2 clinical trials for diabetic neuropathy. However, this year it was cut from the company’s pipeline. ‘It looked promising but then they stopped development, perhaps because of side effects, but we really don’t know why,’ says Safavi. More recently, Safavi and her colleagues in the US and Denmark reported venom-inspired SSTR4 agonists that provide relief to postoperative and neuropathic pain in mice, highlighting their potential as drug leads for peripheral pain.
She is also investigating a deep-water snail venom peptide that activates human neurotensin receptor, also a GPCR. ‘We don’t know if its inhibiting pain in the fish,’ says Safavi. ‘If you give that toxin centrally in humans, in dogs or in rodents, you get very potent pain inhibition.’ There has been interest from companies in this receptor for pain. A group at Duke University reported on a small molecule (SBI-810) designed to target neurotensin receptor 1 in the brain and switch on a signal linked to pain relief.
Beyond cone snails
Growing up in New York, Holford enjoyed visiting the Museum of Natural History beside Central Park. ‘I wanted to be a museum scientist but they don’t usually hire chemists,’ she says. Holford began researching terebrids, a group of screw-shaped snails that burrow into sand and predate marine worms. They were tough to collect and getting their venom proved ‘ridiculously hard’, recalls Holford, though structurally different to cone snails.
Holford has switched to cephalopods, focusing on species of cuttlefish, octopus and squid which she can order as embryos from a neighbouring marine lab. Octopus, for example, make venom in salivary glands behind their beak. Some suspect that they, as well as snails, can vary the recipe for defensive or predatory purposes. They are a vastly understudied group, say researchers. They are likely to yield novel compounds with significant potential as starters for drug design and development, according to Brian Fry of the University of Queensland in Australia.
Rather than producing 10 times more toxin, you make two different ones that act at two different sites along the circuit
One advantage is that the genomes of cephalopods have been published. Holford’s lab can knock out major peptide venom genes with Crispr gene editing to see what happens with the rest of the arsenal. AlphaFold now allows for structure prediction from venom peptide sequences. ‘We have the structures, which is much more powerful, because structure dictates function,’ says Holford. Her lab has even been able to characterise the structures of some of the mysterious compounds from terebrid snails, which she will soon report on.
It makes sense to study individual venom peptides, since multiple unknown peptides together would complicate our understanding of cause and effect. Nevertheless, marine venom comes as an assemblage of biologically active compounds that hit multiple targets. ‘We think it’s a synergistic effect,’ says McIntosh. ‘Rather than producing 10 times more toxin, you make two different ones that act at two different sites along the circuit.’ This raises the possibility that venom peptides might one day be investigated and even developed in combinations, which might be especially useful for something as complicated and multifaceted as chronic pain. Combination drugs are now standard in treating conditions such as cancer.
We’ve barely scratched the surface of the wealth of chemical diversity that nature has to offer
The push to hit and modulate one target has not proved very effective for pain, perhaps because pain is so critical to our survival. ‘There’s so much redundancy built into the system that it’s not very often you can block one target and completely shut down pain transmission,’ says Vetter. ‘We’re embracing this idea that maybe we have to come at multiple targets at once and then you get effective modulation of pathological states.’ Evolution has had tens of millions of years to fine tune venoms and find how and when to pull multiple levers simultaneously. Copying it is an emerging idea in pain therapy. ‘There are an almost infinite number of ways to cause pain,’ notes Fry. ‘There are an equally diverse number of venom toxins that activate or block these pathways.’
Optimism has come and gone before. There was a big push on venom peptides around 2018 and 2019, notes Jamieson, but there were clearly problems taking them towards patients. ‘That probably speaks to a lack of understanding of how these molecules interact with the receptor and elicit their pharmacology.’ Pain itself is a tough area for drug developers. Tumour markers or tissue scans can reveal the efficacy of experimental cancer drugs, but there is no validated biomarker for pain. Animals are not highly predictive of human therapeutic responses. The placebo response is also a tougher confounding factor in pain relief and people experience the same pain differently. ‘I’ve had decision makers in industry tell me that you have to be crazy to invest,’ says Waxman. ‘I urged them to invest in pain therapies. Remarkably, some companies have.’
Nevertheless, the stars might be aligning. There’s the GLP-1 success story, meaning that ‘the peptide field is undergoing a huge renaissance’, says Safavi. This could bolster the huge unmet need for pain medications. Then there are emerging capabilities in deducing peptide structure and genetic tools. Plus, natural peptides are a deep reservoir of possibilities, some of which naturally act in synergy in venoms. ‘We’ve barely scratched the surface of the wealth of chemical diversity that nature has to offer,’ says Vetter. Everyone knows that pushing on to the clinic has been a struggle. ‘Marine venoms are fantastic but there are not that many success stories,’ says Safavi. ‘We need more success stories.’
Anthony King is a science writer based in Dublin, Ireland















No comments yet